COVID-19 pandemic
What is COVID-19 (coronavirus)?
COVID-19 is a viral disease that affects the respiratory system.
The World Health Organization (WHO) declared COVID-19 a pandemic on 11 March 2020. As of September 2024, more than 776 million cases have been reported worldwide.
How has MSF responded to the pandemic?
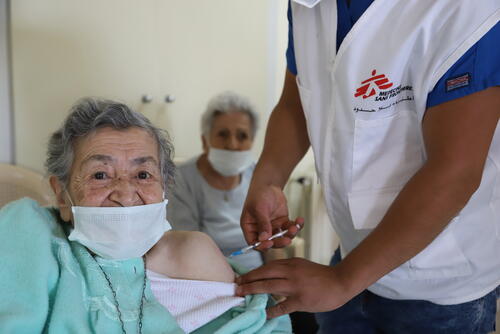
MSF teams have directly responded to COVID-19 in over 40 countries, opening or reopening new projects as they became pandemic hotspots or as the number of cases rises. Since the arrival of the vaccines, we have also delivered and supported mass immunisation campaigns.
During the peak of the pandemic, our COVID-19 response focused on three main priorities:
- Supporting health authorities to provide care for patients with COVID-19
- Protecting people who are vulnerable and at risk
- Keeping essential medical services running
As COVID-19 has spread to countries already facing humanitarian crises, improving access to protective equipment, to COVID-19 tests, to oxygen and to drugs for supportive care, has become essential to the pandemic response. And, since the development of the vaccines, MSF has also campaigned for equitable access and the waiving of patents.
Although COVID-19 cases began to decline in 2022, MSF teams have continued to improve infection prevention and control measures to protect patients and staff and prevent the further spread of the virus. It has been absolutely crucial to keeping healthcare facilities open.
For comprehensive information, including how to protect yourself against the disease, please visit the NHS website on COVID-19.

Help us prepare for the next emergency
COVID-19: Key facts
112,000
MSF CONSULTATIONS FOR COVID-19 IN 2020
15,400
COVID-19 PATIENTS ADMITTED TO AN MSF HOSPITAL IN 2020
6%
WILL REQUIRE CRITICAL CARE
In January 2020, as COVID-19 became a concern, MSF began its first activities in response to the new threat.
As the new coronavirus spread, touching virtually every country in the world, our teams adapted or scaled up ongoing projects and started new activities in many countries over the first six months of 2020.
We committed substantial resources to developing dedicated COVID-19 projects, maintaining essential healthcare in our existing programmes, and supporting ministries of health to prepare for the pandemic. This support was often in the form of training in infection prevention and control, health promotion and organisation of healthcare services.
By the middle of 2020, this training was largely concluded, while most COVID-19-related activities have been integrated into our regular projects, although we maintained some COVID-19-focused projects.
In 2021, further COVID-19-specific activities opened (or reopened) as new waves of infection determined the need to respond. This was - and still is - dependent on the context of a project, the epidemiological situation and the existing local healthcare needs.
With the pandemic affecting almost every nation on Earth, and with MSF operations in more than 70, the consequences of COVID-19 and our response to it have carried vastly from country to country and even project to project.
COVID-19: News and stories