Meningitis
Meningococcal meningitis has a high fatality rate and potentially life-long consequences for survivors.
It's a bacterial form of meningitis, a serious infection of the thin lining that surrounds the brain and spinal cord.
Meningococcal meningitis occurs throughout the world but the vast majority of infections and deaths are in Africa, particularly across the "meningitis belt", stretching from Senegal in the west to Ethiopia in the east.
The infection can progress rapidly, and death can follow within hours of the onset of symptoms.
However, even when the disease is diagnosed early and adequate treatment is started, up to 10 percent of patients do not survive.
Among survivors, 10 to 20 percent are left with lifelong conditions such as deafness, brain damage and learning disabilities.
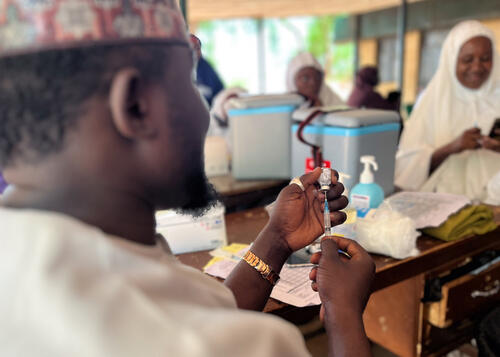
Vaccines are used for prevention and in response to outbreaks.
Meningitis: Key facts
1 in 6
FATALITY RATE OF BACTERIAL MENINGITIS
20%
RATE OF SEVERE COMPLICATIONS FROM BACTERIAL MENINGITIS
26
COUNTRIES IN THE MENINGITIS BELT
Guide to meningitis
What causes meningitis?
Six strains of the bacterium Neisseria meningitidis are known to cause meningitis. People can be carriers without showing symptoms and transmit the bacteria when they cough or sneeze.
Overcrowding and cramped living conditions increase the risk of spreading the disease.
What are the symptoms of meningitis?
When infected people begin to show symptoms, usually one to four days after infection, they often experience sudden and intense headaches, fever, nausea, vomiting, sensitivity to light, and stiffness of the neck.
Although anyone of any age can become infected with meningitis, babies and children are particularly susceptible.
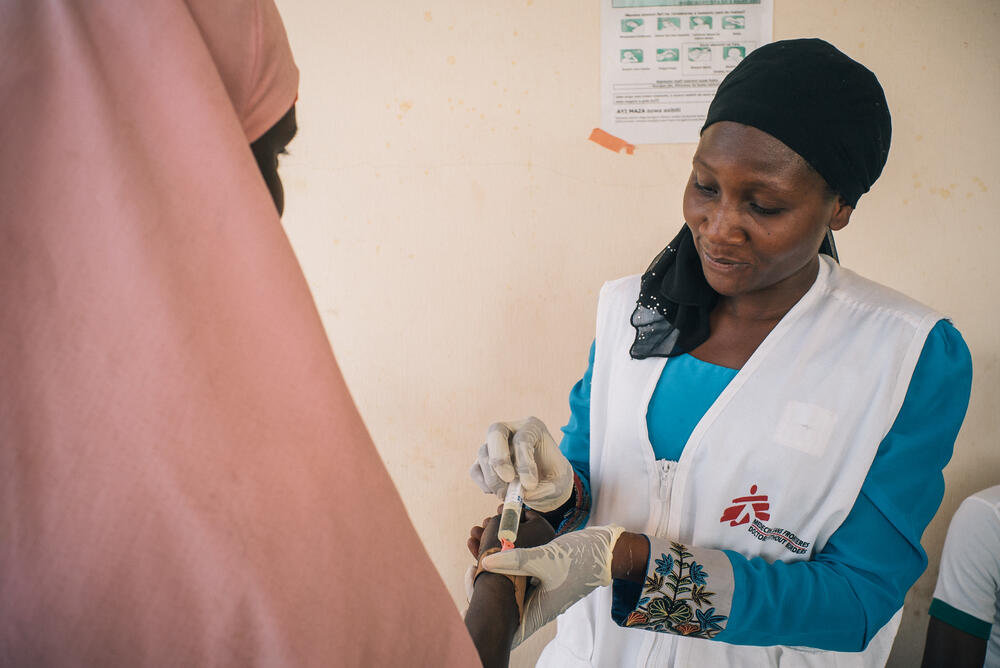
How is meningitis diagnosed?
Diagnosing meningitis in the settings in which we work is often difficult as clinical examination is required - and quickly.
A painful lumbar puncture is needed for the examination of spinal fluid and sometimes the bacteria can be seen under a microscope.
However, the diagnosis is confirmed by growing bacteria from spinal fluid or blood. These diagnostic tests allow for further tests to see how effective certain antibiotics will be for the patient.
How is meningitis treated?
A range of antibiotics can treat the infection, including penicillin, ampicillin, chloramphenicol and ceftriaxone. For meningitis epidemics, in areas with limited health infrastructure and resources, ceftriaxone is the drug of choice.
However, timely mass vaccinations are the most effective means of limiting the spread of epidemics.
In 2010, a new meningococcal A conjugate vaccine was introduced in Africa and, as of November 2017, more than 280 million people had been vaccinated.
According to the WHO, this led to a 58 percent drop in cases and reduced the risk of epidemics by 60 percent. Maintaining high immunisation coverage is expected to eliminate meningococcal A epidemics from the meningitis belt completely.
However, other strains are still causing epidemics. Conjugate vaccines against multiple meningococcus strains (ACWY) are very expensive and in short supply, and are therefore impossible to use for wide-scale preventive campaigns.
Never miss an update
Get the latest news on outbreaks and disease with our email newsletter, Frontline.
You'll also receive our best stories, critical updates and unique ways to get involved.
Meningitis: News and stories