Changing young lives in Lebanon
Thalassemia in the shadow of COVID-19
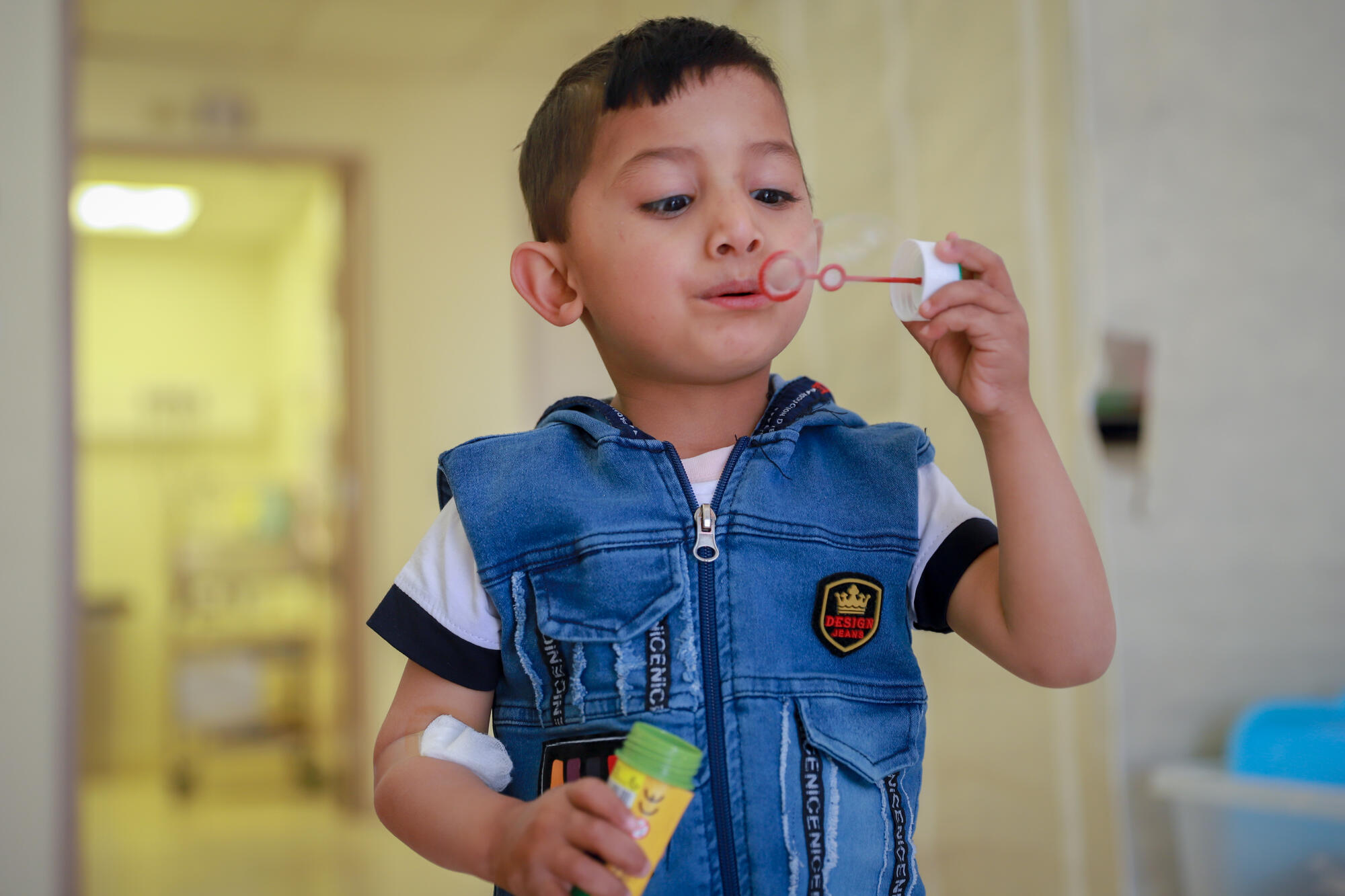
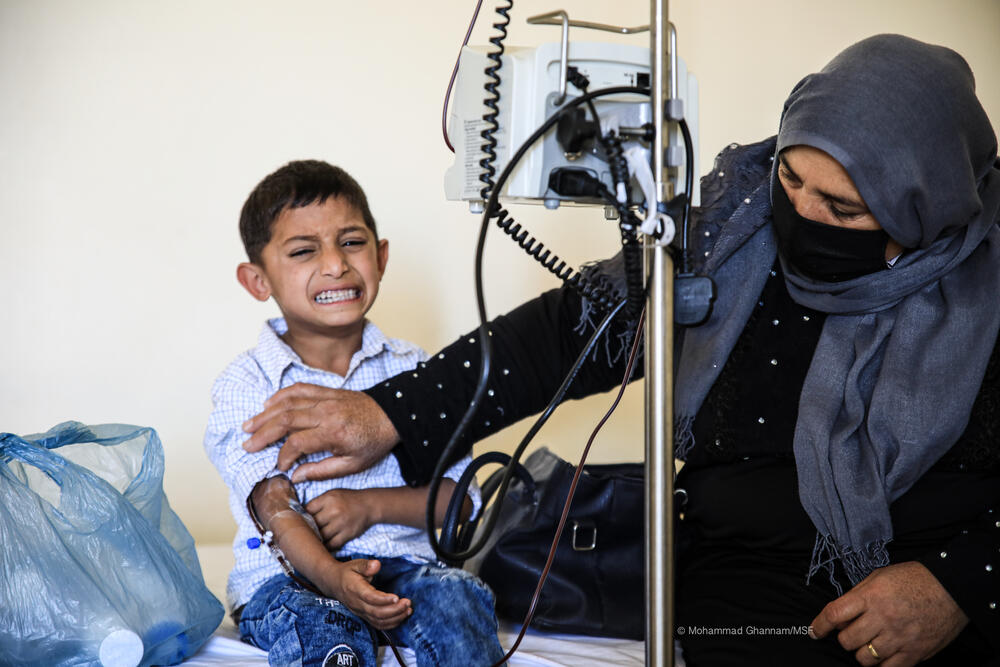
Few parents know the pain of seeing their child suffer as much as Syrian refugee Amira, the mother of two-and-a-half-year-old Mohammad Nour.
Amira lost her elder daughter to thalassemia, a relatively unknown genetic blood disorder that affects people from countries in the Middle East and the Mediterranean basin.
Following the death of her daughter, her younger son was diagnosed with the same disease. Today, Amira has access to healthcare for her surviving child free of charge at Médecins Sans Frontières/Doctors Without Borders' (MSF) thalassemia unit in Elias Haraoui hospital in Zahle, Lebanon.
Nonetheless, their lives are a daily struggle.
Mohammad Nour needs a transfusion every two to four weeks to compensate for the lack of haemoglobin in his blood. “My daughter died, but I want Mohammad Nour to survive,” says Amira.
“But he suffers a lot. He is always crying and always restless. I want him to get better so he can lead his life like other children before it’s too late.”
A costly disease
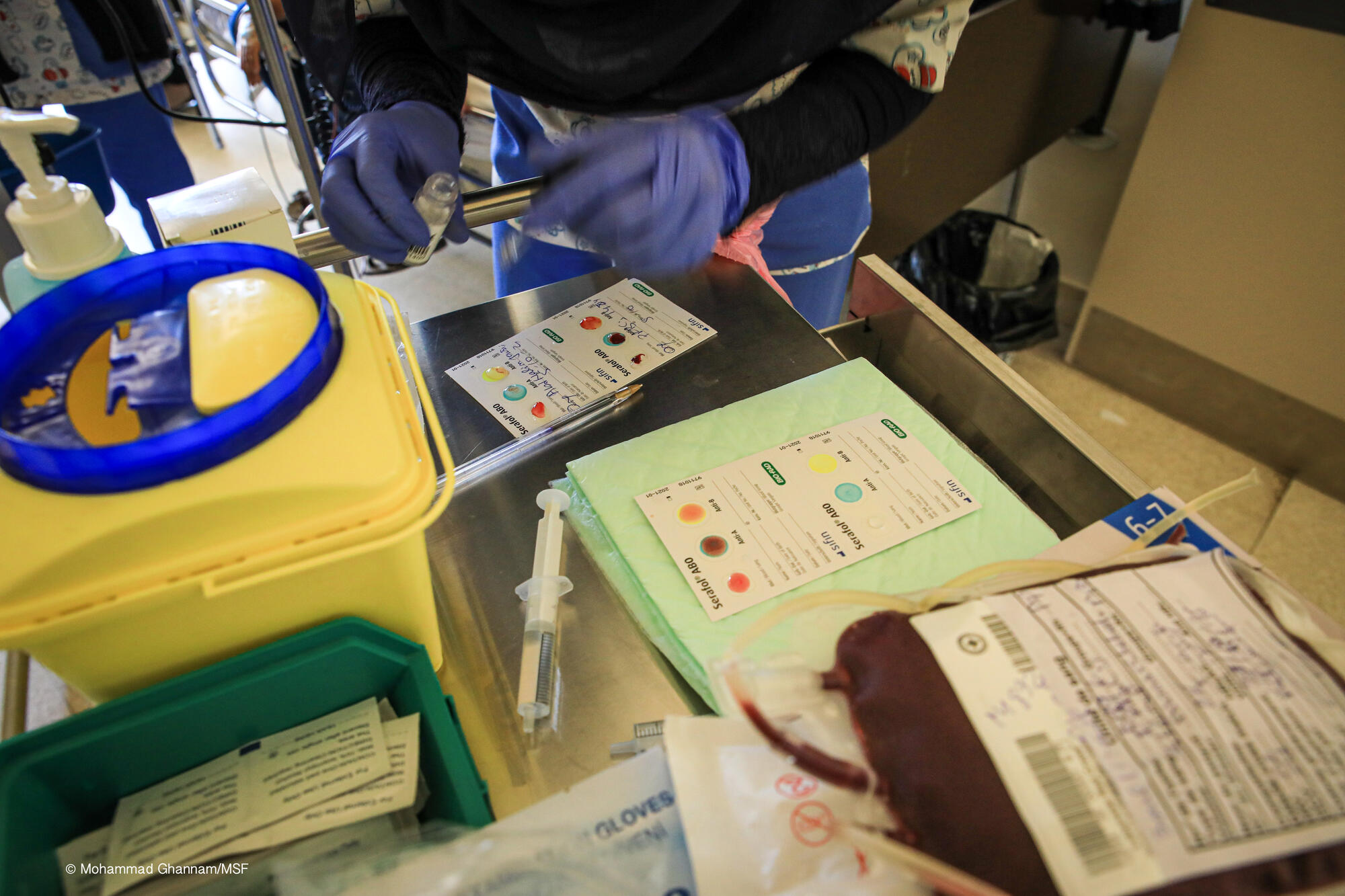
Thalassemia is a dangerous genetic blood disorder caused by an alteration to the genes required to make haemoglobin.
In order to survive, patients with the condition require a demanding treatment of regular blood transfusions as well as chelation therapy – a procedure that removes excess iron from the blood to prevent organ failure.
The condition is found across the Mediterranean basin, including Syria and Lebanon, as well as Pakistan and Afghanistan, where instability has limited access to care.
MSF’s thalassemia unit in Elias Haraoui Hospital provides comprehensive, multidisciplinary care, including diagnosis, blood transfusions, iron chelation therapy and psychosocial support.
Up to £450
COST OF TREATING ONE PATIENT PER MONTH
“Paying the hospital was more important for us even than buying food for the house”
The MSF programme is the only one in the country providing free-of-charge, comprehensive care to children with thalassemia, which is incredibly costly to treat.
Dr Haytham, a paediatric cardiologist at the hospital, says most of the thalassaemia patients he sees are Syrian refugees, with many of them living in makeshift refugee camps in the area around Zahle, though the MSF team also sees some Lebanese children.
The impact of COVID-19

According to the UN, there are nearly 880,000 Syrian refugees in Lebanon. Around 40 percent of them live in the Bekaa Valley, where MSF’s thalassemia programme is located.
The collapse of the Lebanese economy, made worse by the impact of the COVID-19 pandemic, has made it even more difficult for Syrian refugee families to access already overstretched public health services.
The COVID-19 pandemic has impacted families of children with thalassemia in many ways. Community health worker Sami Musa says the main impact has been the increased difficulties in securing blood donations that save thalassemia patients’ lives.
With COVID-19 restrictions in place, roads linking towns are often closed and public gatherings are banned.
“We are trying to get people living in the refugee camps around us to donate blood, but this has been difficult too because people are wary of dealing with medical staff unless they have a medical need.
“They are afraid of us because of our work, some people think we present a COVID-19 transmission risk,” Sami says.
“Every day we explain to people in the communities we work with to convince them that it is safe to donate blood,” he adds.
Thalassemia in the midst of civil war

Thalassemia is a difficult disease for any child to live with. It requires frequent visits to the hospital, sometimes three times per month, recurrent needle pricks, taking daily pills for the rest of their lives, not to mention living with the complications of the disease.
But living with thalassemia is even harder for refugee children in Lebanon, where access to public healthcare is extremely limited for Syrians like Abbas and Youssef.
Now safe after years of suffering, their mother Ammouna recalls why she and her husband had to take their children to Lebanon. They had endured years of bombing when the Islamic State group took over the town of Manbij where they were living at the time.
The armed group did not allow civilians to leave the town – so Ammouna could no longer travel to Syria’s second city Aleppo to buy the drugs her boys needed to bring the iron levels in their blood down.
Then, after the Kurdish-led Syrian Democratic Forces took over, travel became possible again, but blood transfusion services nearly came to a halt.
“So for three years, I had to arrange for the blood transfusions at home,” Ammouna says, adding that she had to ask members of the community for blood donations. “It was a very difficult period,” she adds.
Ammouna and her husband eventually took their children to Lebanon, hoping life would be kinder there. But they quickly discovered the prohibitive costs of healthcare in Lebanon’s private clinics.
They were on the verge of giving up and returning to Syria when they found out about the MSF programme at the Elias Haraoui hospital in Zahle, which provides comprehensive care for thalassemia patients free of charge.
“Here at the hospital, my boys receive the transfusions and medication they need,” says Ammouna, who works on a local farm for a daily wage, and whose husband is a carpenter. “We’ve been coming here for some three years now.”
The Beirut blast

The August explosion that obliterated Beirut port has made the situation for the MSF programme even harder. When Sami and his team approached potential donors in the aftermath of the blast, many said they had recently donated for the injured.
The dearth of donors poses an even greater risk for thalassemia patients with rarer blood types such as O negative and AB negative. “We are expanding the areas we target for donors. We will keep fighting,” Sami says. “This is the only way.”
Gharam, MSF’s external relations supervisor for the Zahle programme, says that one of the ways she and her colleagues ensure that enough blood donations are made is by providing transportation for donors to Lebanese Red Cross centres that are working with MSF.
“Blood transfusions done in hospitals are very costly,” Gharam says, adding that refugee and other vulnerable families already have a hard time putting food on the table before they consider any medical costs.
The MSF-run programme at the Elias Haraoui hospital in the heart of Zahle currently provides treatment for 96 children living with thalassemia.
“We increased the number of the children we treat from 74 up to 96 in November,” says Dr Layal, MSF’s medical activity manager for the programme. “We wished we could do more to respond to the needs but we are limited by the very high price of the thalassemia drugs.”
‘Like any other child’
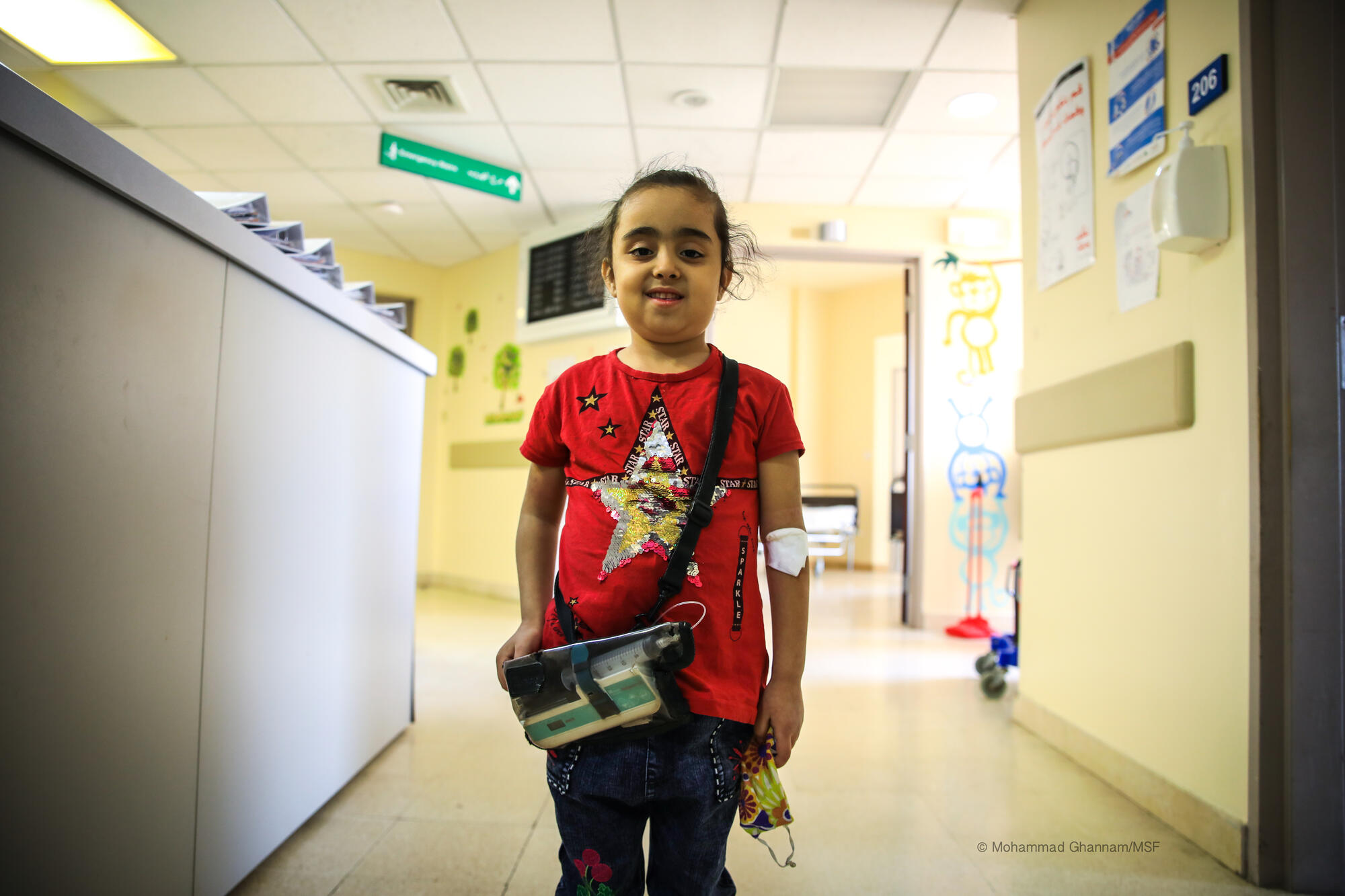
War was raging in Syria when Hani and his wife fled to Lebanon. Soon after their first child Dalal (above) was born, a doctor diagnosed her with thalassemia. “That was the beginning of our nightmare,” Hani says.
For every blood transfusion that Dalal needed, Hani and his wife had to pay over £145 in hospital fees alone.
“Paying the hospital was more important for us even than buying food for the house,” he says, adding that it was excruciatingly difficult, even humiliating, to find a donor each time to secure the blood required for every transfusion.
The father, who earns an average £220 a month painting houses, describes one incident when his daughter was so ill that she had to be hospitalised.
When her condition improved, the hospital asked him for £1,460 in fees – a sum he and his wife simply could not afford.
“I left my ID at the hospital so I could get her discharged, and sold all my belongings, even though that raised only about half of the sum. I borrowed money from everyone I knew, but even that was not enough.
"I ended up living without an ID for a full year – you can imagine how difficult, how risky that is for a Syrian refugee in Lebanon,” Hani says.
Eventually, life took a turn for the better in 2018 when he found out about the MSF programme. Dalal, now seven years old, receives regular follow-up free of charge.
“Now I see my beloved Dalal smiling and playing like any other child. I am happy she is receiving the best possible treatment for her illness, offered by the kindest medical staff I have met in my life,” Hani says.
As refugees in Lebanon, the family still faces a long, tough road ahead. “But I am so happy and grateful for what we have now,” he adds.
MSF in Lebanon
In its heyday, Lebanon was referred to as the Switzerland of the Middle East because of its financial power and diversity. Today, the country is struggling to cope.
Civil war in Syria has put a huge strain on its neighbours, including Lebanon, which now hosts over a million refugees – the most per capita in the world.The devastating explosion that struck Beirut in August 2020 has put the country under extreme strain.
Médecins Sans Frontières/Doctors Without Borders (MSF) has been working Lebanon since 1976, when we began our response to the 15-year civil war. Today, we are helping refugees, many of whom live in deplorable conditions with their most basic needs unmet.
Our teams provide these communities with free, quality medical assistance, including treatment for non-communicable diseases, sexual and reproductive healthcare, mental healthcare and maternity services.
In 2019, in a year marked by mass anti-government protests across Lebanon, we continued to provide general and specialist healthcare to host, migrant and refugee communities.