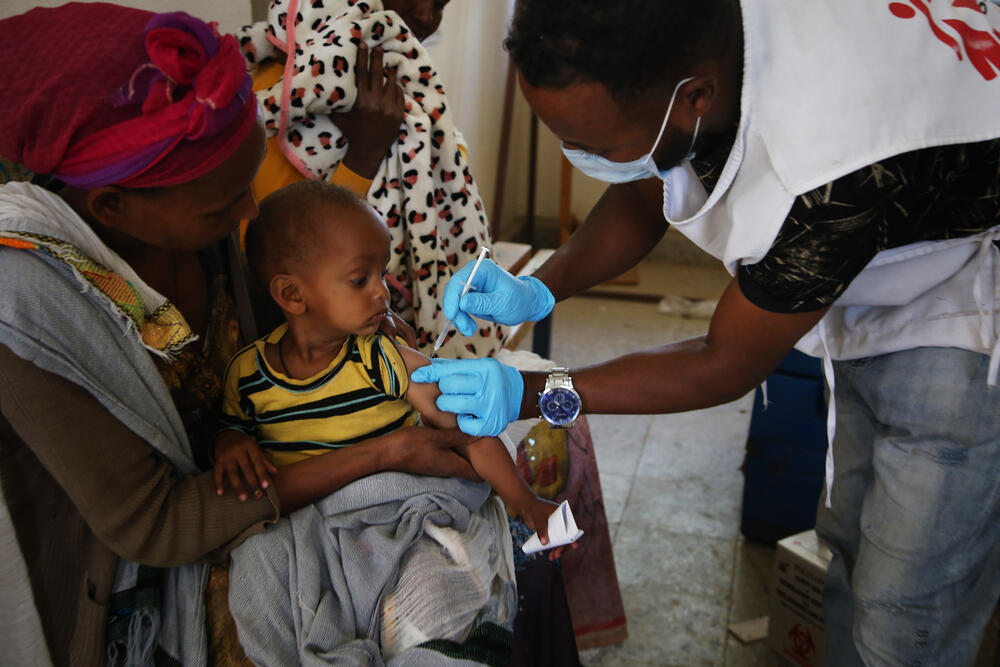
Photostory: Reaching the forgotten communities of the Tigray crisis
How MSF teams in Ethiopia are taking treatment to remote villages cut off by violence

As the conflict in Tigray continues, emergency teams have been deployed to cities across northern Ethiopia to help the six million people hit hard by the crisis.
At the same time, the huge numbers of people living in the region’s remote and mountainous rural areas have been cut off from essential healthcare for six months – almost invisible to the outside world.
Now, MSF's mobile clinics are delivering aid to people still living in fear.
When a small MSF mobile team reached the remote village of Adiftaw for the first time, they found the health post had been looted and partially destroyed.
Medical files, broken equipment and emptied medicine packets were scattered across the floors of every room. None of the beds had mattresses and there were no staff.
This was nothing new and echoed their experiences on almost every visit to a new place anywhere across Tigray.
Triage
In the months since clashes started in November 2020, the 10,000 people living in and around Adiftaw have been unable to see a doctor or be referred to a hospital.
Soon after the MSF team had cleaned up the health post and opened a temporary mobile clinic, dozens of people showed up, arriving slowly but steadily from all directions.
Mostly they were mothers carrying small children wrapped on their backs. Young men carried an elderly man who was apparently sick with malaria on an improvised stretcher. Elderly women appeared, their bodies aching from chronic conditions.
However, the medical staff had to focusing on children, pregnant women and people needing emergency care. Eventually, the team were unable to see any more patients as there simply was not enough time or staff.

Living in fear
Beyond healthcare needs, the consequences of the violence had hit people in Adiftaw very hard.
Some farms were still occupied by soldiers, the mill no longer functioned and the water system was deliberately broken.
Instead, people had to walk for hours to fetch water from a river that they said was a source of diseases including diarrhoea.
More than 100 houses had been burnt or damaged by shelling and other violence, and dozens of residents had reportedly died or gone missing, with some still hiding in the mountains.
“When we arrived in Tigray in late 2020, we found that the health system had almost completely collapsed,” says MSF emergency coordinator Tommaso Santo.
“Once we had set up support in hospitals in big towns such as Adigrat, Axum and Shire, it seemed essential to us to reach the more remote areas where people’s needs are greater.”
MSF emergency teams are now running mobile clinics in around 50 different locations.

Help us prepare for the next emergency
“Every time we get access to a new site, we send in a small team that can provide a basic package of medical services,” says Santo.
“We are finding people with very little access to drinking water and food distributions, and who cannot do commercial activity due to some markets being closed. Many people are still living in fear in a situation of insecurity.”
Malnutrition
Our teams are seeing large numbers of pregnant women with medical complications, some of whom are malnourished, which can increase the risk of disease and death during pregnancy and childbirth.
While child malnutrition rates vary, moderate acute malnutrition has been on the rise across Tigray in the last months, with many families only able to eat one basic meal a day.
However, some areas are now showing levels of severe acute malnutrition well above the “emergency threshold” such as in the outskirts of the city of Shire and in Sheraro.

A healthcare system in ruins
Before the conflict, Tigray had a well-functioning and well-equipped healthcare system that was among the best in Ethiopia. Health centres in rural areas covered people’s basic needs and were connected to the main hospitals through a fleet of ambulances that transported patients needing specialist treatment.
One such rural health centre was in the town of Sebeya and used to serve a community of around 17,600 people.
“Services here were good,” says Fatimah*, a 27-year-old woman from Sebeya.
“I gave birth to all my four children here. If the health staff didn’t have the capacity to do something, they’d send you to Adigrat. I never had to go, but other patients would be taken there in the ambulance.”
Now, the ambulance is missing and Fatimah, who is seven months pregnant, will not be able to deliver her fifth baby at this health centre.
Sadly, just metres away from where she waits for an antenatal consultation with the MSF medics, the centre’s delivery room – where 50 women used to give birth each month – lies in ruins, destroyed by rockets in mid-November.
“These days women are delivering at home,” says Solomon*, a health worker.
“Even if the birth goes well, newborns face the risk of dying. People with chronic conditions such as HIV, tuberculosis or diabetes are suffering due to the interruption of their medication. Children are dying due to pneumonia and malnutrition.”

A drop in the ocean
For the residents of Sebeya, the resumption of basic medical services through a mobile clinic may be a positive step, but it is still a mere drop in the ocean. Most people here have lost their livelihoods and experienced months of harsh conditions, if not direct violence.
“I was a merchant before the crisis,” says Mariam*, as she waits for her antenatal check-up.
“I had a shop selling coffee, sugar and cleaning materials, but now it is closed. It was looted after we fled the town to seek refuge. I was in hiding for four months.
“We never thought the conflict would hit us. I never thought I’d find myself without food and having to hide in the bush.”
Over these few days, close to 300 medical consultations were carried out in Sebeya and Adiftaw by MSF’s mobile teams.
Apart from sexual and reproductive health issues, the most common conditions seen, particularly among children, were malnutrition, pneumonia, diarrhoea and skin diseases related to poor living conditions and unclean drinking water.

Get closer to the Frontline
Get the latest news, stories and updates, straight to your inbox.
Beyond the towns and cities
“We try to prioritise the areas where we should continue responding,” says Santo.
“And we try to increase the package on offer: it might be family planning, antenatal consultations, vaccinations or other services, none of which have been available for months.”
There is also a clear need in rural areas for treatment and care for survivors of sexual violence, which has been a recurrent feature of the conflict.
Over recent months, MSF-supported hospitals in the cities have been seeing rising numbers of women seeking psychological support from traumatic experiences and the termination of unwanted pregnancies. More needs to be done to expand people’s access to these and other critical support services.
While more humanitarian organisations have sent teams to Tigray, especially since February, the response on the ground is still extremely limited as it hardly ever extends beyond the larger towns.
“Rural areas are often left without any kind of assistance and in recent weeks access for humanitarian organisations to various parts of Tigray has been further constrained,” says Santo.
“There is an urgent need to scale up humanitarian assistance and to expand its reach.”
*Names have been changed to preserve anonymity
MSF and the Tigray crisis
Tens of thousands of refugees have fled the Tigray region of Ethiopia after fighting erupted in early November 2020.
Our teams began triaging and treating war-wounded people on 5 November in the Amhara region of Ethiopia, and are also providing emergency medical care to people who have fled across the border into Sudan.
People fleeing the violence are in urgent need of medical care, shelter, water and food.
As of the end of March 2021, MSF teams are supporting five hospitals in the region and are running mobile clinics in dozens of locations.