Ebola in Uganda: “Our game-changing treatment centres will save more lives”
Infectious disease specialist Ruggero shares his traumatic experiences of treating Ebola, and the simple innovations that will improve survival rates in Uganda’s outbreak.
I worked continuously for Médecins Sans Frontières / Doctors Without Borders (MSF) between 2003 and 2017. Infectious diseases are my speciality, so I’ve worked in different outbreaks, including cholera and Ebola, as well as in malnutrition crises.
In my long history with MSF, I think the experience that touched me the most was the 2014-16 Ebola outbreak in West Africa.
I was sent as medical coordinator to open a project in Monrovia, the capital of Liberia, at the peak of the outbreak. It was really a very traumatic experience, and very hard to provide a good level of care as we were submerged by patients.
We saw more than 20,000 patients in one year when previously there were only 2,000 in each of the 20 previous years. However, it was a privilege and scientifically very stimulating to work in this outbreak and try to find life-saving solutions that were practical.
“This virus is dangerous and you need to be careful, but the PPE reduces the humanity that we can show to a patient”
It reminded me of older times when I was treating HIV/AIDS.
I was a young doctor then, specialising in HIV. We were seeing all these young people dying, then sitting up all night talking about what we could do to improve the care. Again, it was traumatic because we had 50 deaths per day, something like a war. We worked hard to try and find clinical solutions.
Never miss an update
Get the latest news on outbreaks and disease with our email newsletter, Frontline.
You'll also receive our best stories, critical updates and unique ways to get involved.
Tackling the Uganda outbreak
Right now, Uganda is in the middle of an Ebola outbreak. And, I have also returned to working for MSF.
Recent large outbreaks of Ebola have been caused by the Zaire strain of the virus and were followed by the development of vaccines and treatments. However, this outbreak is being driven by a rarer variant known as the Sudan strain.
I am now at the epicentre of the outbreak, where we have set up an Ebola treatment centre at Mubende Referral Hospital.
There were originally two areas: one for confirmed patients and one for suspected cases. However, the recent peak in infectious means we have had to adapt to treat more confirmed Ebola patients.
To both treat patients and prevent the spread of the infection, you find yourself doing tasks that are beyond a doctor’s usual scope of practice.
I do ward rounds but also set up intravenous lines, clean up patients, provide nursing care, clean the area and also act as a watchman.
We have to focus on the things that have the most impact. Medical care, but also the dignity of patients.
This disease is very serious.
When entering the body, the reaction is massive and progresses quickly. Patients might be walking a bit when they enter the treatment centre, but then they deteriorate fast.
MSF has been supporting #Uganda's Ministry of Health in its #Ebola response since September 2022. One part of our work here has involved building Ebola Treatment centres (ETCs) where we can provide high-quality care.
— MSF East Africa (@MSF_EastAfrica) November 10, 2022
What does an ETC look like? Walk with us 👇🏽 pic.twitter.com/KBcso6VCwG
Game-changers
MSF has valuable expertise and experience in responding to Ebola outbreaks. However, we have worked to improve how our treatment centres work. This is so that medical staff can move about more easily and work more efficiently.
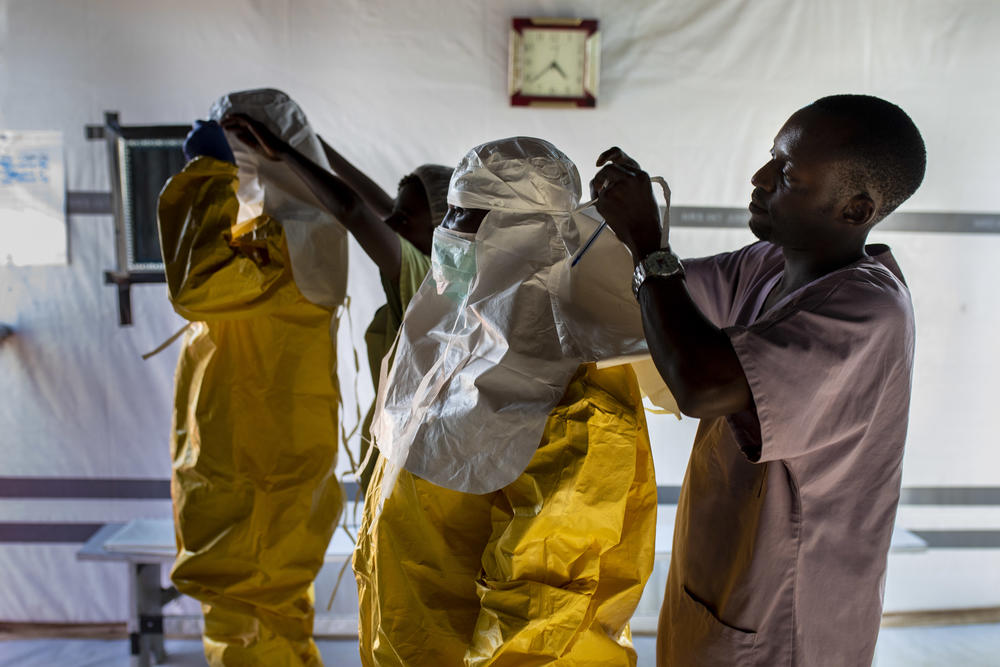
The problem is the thick, high-level Personal Protective Equipment (PPE) usually worn when dealing with Ebola. We need to have clear visibility of patients and be there 24/7. But, with this PPE, you cannot do it.
On one hand, this virus is dangerous and you need to be careful, but the PPE reduces the humanity that we can show to a patient. It also limits our medical interventions. For example, if you have to find a vein in a patient’s arm, it’s not easy in the thick gloves.
Then there’s the sweat. The heat inside this PPE means there are limits on how long you can wear it. I’m also getting older and need to wear glasses, but you can’t inside the suit.
So, we have worked to get new and improved PPE that is lighter and allows you to be with patients for much longer.
However, the real game-changer is the new structure of the treatment centres themselves. They now have see-through sections, meaning patients can be monitored every second of the day from the outside. It’s a great concept.
Medical staff will be able to see a person’s vital signs and keep up with the virus. We know how the disease progresses. So, when we see that we need to act, we can act fast.
If I see that a patient’s oxygen levels are going down, we can put on the new PPE and enter the room to give oxygen. If their heart rate is changing, if they need fluids. Whatever it is, we can intervene in a targeted and timely way.
Working with communities
A big issue is the late arrival of patients, coming when the disease has already progressed. It’s very challenging to treat. But, if I can get you on day two or three of the disease, the studies show that your chance of survival increases.
This is key to surviving Ebola.
It’s very hard when you realise that your patient is not going to make it. You know you can try your best, but you also know the severe symptoms and know the chances. I remember once treating a very agitated patient like this. He took my hand and asked, “Please stay with me”. I realised he was going to die.
So, our outreach team works with communities to improve early admissions – speaking to people about our services and contract tracing suspected and confirmed cases.
This is the other side of the story.
Every time you have a survivor leave the centre… it is a joy. We had six survivors leave the other day and it was a party! It is a coping mechanism. Every time someone recovers from Ebola, you say “Ahhh”.

Help us prepare for the next emergency
MSF and Ebola
Ebola is one of the world’s deadliest diseases.
It is a highly infectious virus that can kill up to 90 percent of the people who catch it, causing terror among affected communities.
Ebola is so infectious that patients need to be treated in isolation by staff wearing strict protective equipment and clothing.