Cameroon: The community-led team reaching people cut off by violence
Update: MSF ambulance attacked
In the early hours of 4 February, an MSF ambulance was fired on by armed men while responding to a call in Muyuka, South West Cameroon. The ambulance was hit and a nurse was injured.
We condemn this attack on our colleague and a clearly marked ambulance. Healthcare facilities, including ambulances, are not targets.
Following this attack, a second ambulance was dispatched to pick up the patient who is in critical condition and now receiving medical attention. Our colleague is also receiving medical attention and is currently recovering from their injuries.
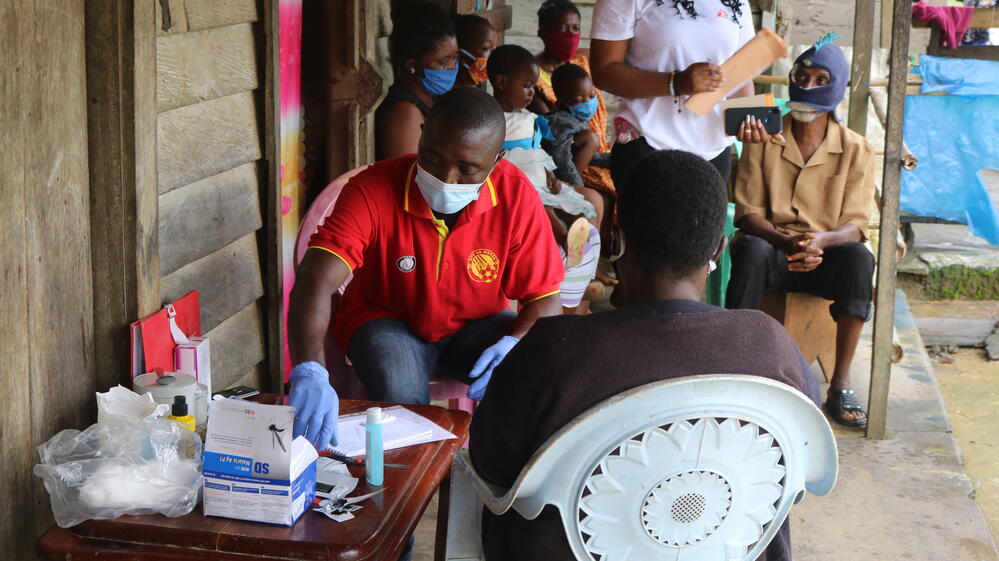
Around a dozen adults and children are waiting patiently for their check-ups. Sitting behind a small table, Etienne Esua listens to patients, dresses wounds and pricks fingers to perform rapid malaria tests.
“When a test shows that a person has malaria but the symptoms are not severe, I treat the patients with drugs,” he says.
The consultations are taking place on the veranda of an ordinary house in a village in the South West region of Cameroon.
Etienne is not a medical professional, but a community volunteer trained by Médecins Sans Frontières / Doctors Without Borders (MSF) to provide primary healthcare to some of the region´s most vulnerable and hard-to-reach communities.
Armed violence
For the past four years, Cameroon´s North West and South West regions have been rocked by armed violence between government forces and non-state armed groups, which has displaced more than 700,000 people.
“Community health volunteers are the bridge between the healthcare facilities that we support and vulnerable communities"
The humanitarian needs are huge. Displaced communities face difficulties accessing basic services, including healthcare, and the crisis has severely affected the public health system.
Many healthcare centres have closed or no longer function, medical workers and facilities are being directly targeted by violence, and insecurity is hindering the supply of drugs and medical equipment.
Given this high level of insecurity, humanitarian organisations like MSF face serious problems trying to reach displaced communities, who often hide in the bush for their safety.
Community care
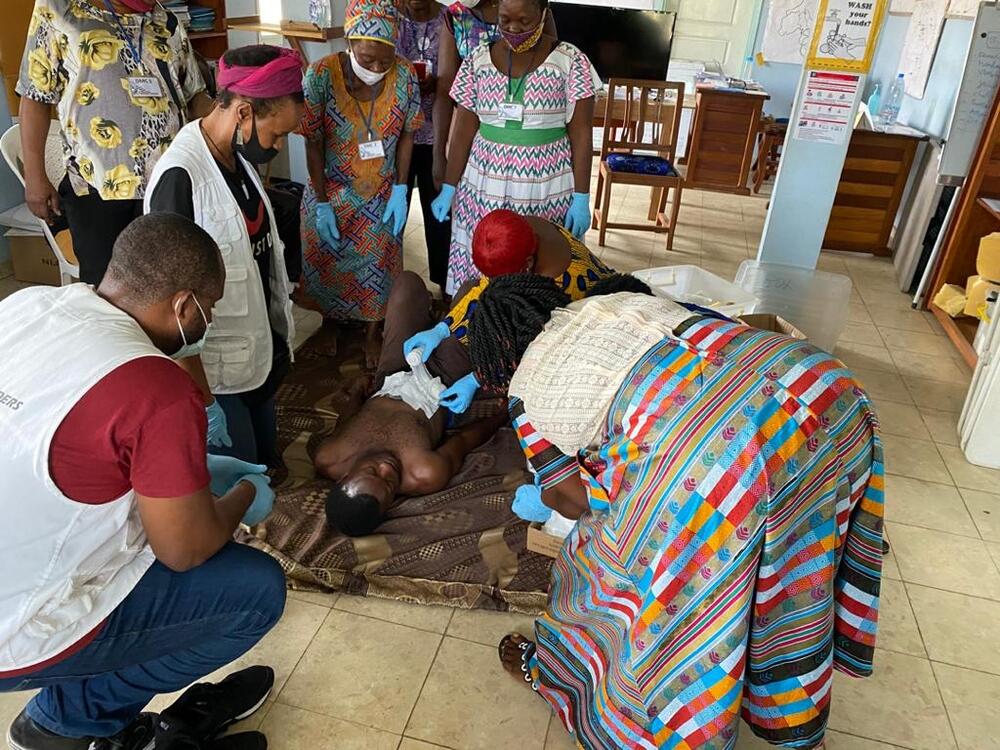
To provide medical aid in such challenging conditions, MSF has set up a decentralised model of care, also known as DMC, in the South West and North West regions which is delivered directly in the community, by the community. It relies on volunteers like Etienne.
“Community health volunteers are the bridge between the healthcare facilities that we support and vulnerable communities that don´t have access to these centres," says MSF coordinator Yilma Werkagegnehu.
"This is either because they are displaced, because healthcare facilities are closed or because they can´t afford to pay for medical services.”
MSF currently works with 106 community volunteers in several health districts near the towns of Mamfe and Kumba in the South West region.
Similar services were conducted in the North West until December 2020, but have been put on hold following a decision by the authorities to suspend MSF activities in the region until further notice.

Help us prepare for the next emergency
The first line of healthcare
Community health volunteers have been recommended and selected by community leaders and trained by MSF to detect and treat conditions like uncomplicated cases of malaria and respiratory tract infections, malnutrition and diarrhoea.
They also learn how to carry out health education activities to prevent people from getting sick, and how to recognise signs of sexual abuse and psychological distress.
While they might not be medical professionals, these volunteers are still trained to adhere to medical ethics, and to treat those in need, regardless of background.
The community health volunteers are paid incentives for their work and receive backpacks filled with medicines. They meet regularly with MSF supervisors to discuss their work, get advice and share medical data. Their backpacks are refilled before they return to visit remote communities, often walking for several hours a day.
In 2020, these volunteers provided more than 150,000 free medical consultations in the South West and North West region.
Complicated cases
If a treatment is beyond their capacity, community volunteers can refer patients to MSF-supported healthcare facilities where they can receive free treatment.
This might include children with severe malaria, women with complicated pregnancies, survivors of sexual violence or patients with intentional injuries.
“Our community volunteers are sometimes harassed by armed men… we need everyone to understand that community volunteers and ambulances provide a much-needed lifeline”
One of the referred patients is a seven-year-old girl named Dorcas. She is sitting on a bench next to her mother outside the MSF-supported Presbyterian General Hospital in Kumba, South West region. Her left leg is in a cast.
“The girl was injured in a traffic accident and was referred to the hospital by one of our community volunteers,” says MSF doctor Guisilla Dedino.
“She was assessed in the emergency room and was diagnosed as having an open fracture of the left leg. A surgeon from MSF operated on her, and she is making progress with the fracture showing good signs of healing.”
Ambulance teams
Travelling from remote villages to healthcare facilities is a major challenge for many people, due to insecurity, bad road conditions and lack of transport.
MSF offers a free, 24-hour ambulance service that operates seven days a week, collects eligible patients at designated pick-up points and takes them to MSF-supported healthcare centres and hospitals.
MSF in Cameroon: In numbers
4,050
EMERGENCY ROOM ADMISSIONS BY MSF IN CAMEROON IN 2024
89,100
OUTPATIENT CONSULTATIONS BY MSF IN CAMEROON IN 2024
1,640
SURGICAL INTERVENTION BY MSF IN CAMEROON IN 2024
Where we cannot go, MSF provides money for public transport so that patients can reach healthcare facilities or pick-up-points. However, managing a decentralised model of care and ambulance service is not easy in such an insecure environment.
“Our community volunteers are sometimes harassed by armed men,” says MSF emergency coordinator for the South West region, Paulo Milanesio.
“We are in constant dialogue with different stakeholders to guarantee their safety. We need everyone to understand that community volunteers and ambulances provide a much-needed lifeline for vulnerable communities who would otherwise be deprived of medical care.”
MSF in Cameroon
Created in 1961 by the unification of a British and a French colony, and home to nearly 24 million people, Cameroon is often referred to as “Africa in miniature” because of its geographical and cultural diversity. However, the central African country has struggled to find peace and unity.
In 2019, armed conflict intensified between the government and separatist non-state armed groups from the English-speaking communities in the Northwest and Southwest regions, while insecurity and violence in neighbouring Nigeria continued to push thousands of Nigerian refugees across the border.
Médecins Sans Frontières/Doctors Without Borders (MSF)'s work in Cameroon has focused on responding to endemic and epidemic diseases, and caring for displaced people and those affected by violence.