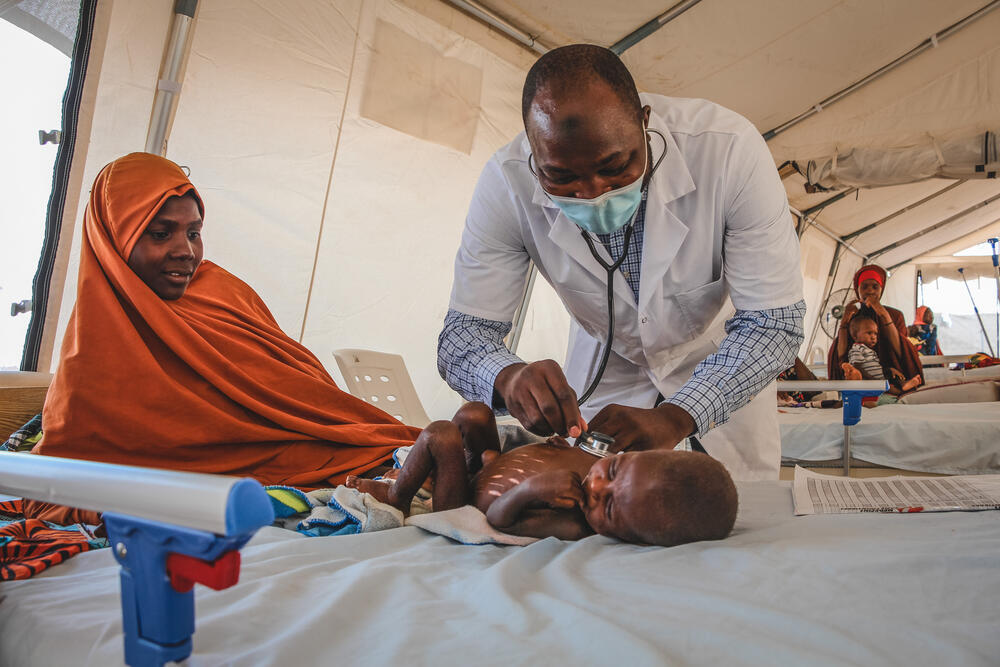
Malnutrition in Nigeria: “We needed to act fast”
When a little girl arrives in critical condition, the team know they must act quickly to save her. But she’s one of thousands of children affected by a malnutrition crisis in the region. Medical Activity Manager Dr Bukar Galtimari explains how the team is working to save lives.
By the time the mother arrived at our hospital in Maiduguri, her little girl was unconscious.
They had travelled a long way. Three or four hours in a shared car, stopping and waiting at each military checkpoint along the way, as the little girl became progressively more unwell.
When they finally reached us, the triage nurses rushed them through to the emergency room. Her blood sugar test showed she was hypoglycaemic (lower levels of blood sugar than standard), which was no surprise: she looked undernourished, and her hair came away easily from her head.
A measurement of her mid left upper arm showed how wasted her body was. She had severe acute malnutrition.
Her name was Hafsat* and her mother told us that she was five years old.
We gave Hafsat glucose, and she started to open her eyes.
“With Hafsat admitted to the hospital, our team worked quickly to get a diagnosis and start her on the right treatment. The tests showed she had sepsis; a life-threatening condition caused by infection. However, that wasn’t all…”
Malnutrition crisis
In Nigeria it’s estimated that over 30% of children under the age of five have stunted growth caused by chronic malnutrition – where they don’t get enough to eat over a long period of time. This is one of the highest rates in the world. For severe acute malnutrition, the number is estimated at around two million children, with only 20% having access to care and treatment.
The “peak” malnutrition season is from April to November, when supplies of food from the previous year’s harvest start to run out. However, in our region there are other factors driving the crisis…
Maiduguri
Maiduguri is the capital of Borno State, in the northeast of Nigeria. Many of our patients have come to the city to escape armed conflict and insecurity in the region. Far from their homes and livelihoods, they don’t have the means to earn a living. Even for locals, the security situation means it’s often not safe for people to farm their lands.
Families are also hit hard by the high rate of inflation. A sack of rice now costs 35-38,000 naira (about $80/£65). A sack of beans you could previously buy for 6,000 or 7,000 naira (around $14 / £11) now you cannot even get for 30,000 (about $65/£53). These are huge amounts. People can’t afford to feed their families.
Access to health services also has an impact. Breastfeeding can prevent younger children from becoming malnourished, but without quality maternity care, many families don’t have the correct information about this.
Meanwhile sick children are more likely to become malnourished, and children who are malnourished are more likely to become ill. They’re also more likely to die from their illnesses, so access to health care and vaccines is also vital.
An accurate diagnosis
With Hafsat admitted to the hospital, our team worked quickly to get a diagnosis and start her on the right treatment. The tests showed she had sepsis; a life-threatening condition caused by infection. However, that wasn’t all. After talking to Hasfat’s mother about her daughter’s health, we also suspected pulmonary tuberculosis.
Malnutrition weakens the immune system, leaving people more vulnerable to infectious diseases. We took a sputum sample from Hasfat and sent it to our in-house lab team for analysis. The results confirmed our suspicions: Hasfat tested positive for tuberculosis.
Adapting fast
I’ve worked for MSF in Maiduguri since the malnutrition project here first opened in 2017. We started with an outpatient service and a few inpatient beds for the sickest children. But the needs were so great that soon we had to scale up: becoming a 120-bed hospital.
Last summer, during peak season, the malnutrition rates reached emergency levels. More and more critically ill patients kept arriving.
We needed to act fast. In a matter of three days, we had scaled up again. We created a ward in a tent to increase our bed capacity.
And because MSF is independent, we didn’t have to wait months for approval from funders to act. Over the following weeks, our 120-bed hospital grew to 350 beds.
Hafsat spent 16 days at the hospital.
Ongoing care
Left untreated, tuberculosis is life-threatening, but we have a well-established TB programme and were able to start Hasfat on treatment immediately.
Once she was well enough, her family took her home, but she continued to come regularly to receive special therapeutic food and monitoring from our outpatient malnutrition team, and then head to our designated TB doctor.
If all goes well, Hafsat will complete her TB treatment within six months.
When they come to see the follow-up team, Hasfat’s family often stop into the ER too, saying “Doctors, see your child!”
It always makes all of us who were involved in her care happy, because just by looking at her we can see that she is gaining weight and her health has improved.
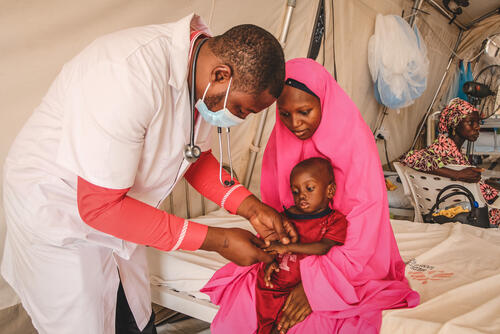
Increasing numbers
Last year, we treated 8,071 in-patients, an increase of 144% on the year before. We not only had to increase the number of beds, we also hired extra staff, trained them, brought in additional supplies and tried to look after the wellbeing of our team so they could provide the best care possible to thousands of very ill, very malnourished children.
At the start of this year, with the peak season still months away, we were already admitting double the typical number of patients. Right now, it’s manageable. But the numbers will only increase, so we must be ready.
*Name changed
MSF in Nigeria
Nigeria With over 190 million inhabitants, Nigeria is the most populous country in Africa.
Nigeria also has one of the fastest-growing economies, which is based primarily on the petroleum industry. However, a decade-long conflict has devastated the northeast of the country. Thousands have been killed and nearly two million people have been uprooted since fighting broke out between the military and non-state armed groups.
Médecins Sans Frontières/Doctors Without Borders (MSF) has been responding to disease outbreaks and emergency health needs in Nigeria for many years, focusing on maternal and paediatric healthcare throughout the country and scaling up our activities in the northeast as vast numbers of people caught up in the conflict depend on aid to survive.