Ebola in Uganda: Four things you need to know about the outbreak
On 20 September, Uganda declared an outbreak of the Ebola virus.
The Ugandan Ministry of Health has since confirmed 64 cases, reporting 25 deaths from the deadly disease as of 19 October.
Médecins Sans Frontières / Doctors Without Borders (MSF) is now working with authorities to set up an initial emergency response to help stop the virus from spreading further.
The Sudan strain
MSF has vital expertise from responding to various Ebola outbreaks over the past decade, including the huge West Africa outbreak from 2014-16 and in the Democratic Republic of Congo (DRC) from 2018-20.
These epidemics were caused by the Zaire strain of the Ebola virus and were followed by scientific advances, including the approval of two vaccines and an antibody treatment for the disease.
However, the current outbreak in Uganda is caused by a relatively rare variant of the virus known as the Sudan strain. This raises several medical and operational challenges for teams on the ground.
Tackling the spread of the disease now requires rapid development of an effective detection and treatment programme in a country that has been relatively free of epidemics for the past decade.
Here are four important questions and answers about the Ebola outbreak in Uganda.

Help us prepare for the next emergency
Explained: Ebola
Ebola is a serious and often deadly virus with a mortality rate of up to 90 percent.
Initial symptoms are similar to those of many other illnesses: sudden onset of fever, fatigue, muscle aches, headache and a sore throat. These may be followed by vomiting, diarrhoea, a rash, kidney and liver failure and, in some cases, internal and external bleeding.
First discovered in 1976 in the DRC, there are several variants of the disease with the Zaire strain being the most common over the past decade. To date, there have been seven outbreaks involving the rarer Sudan strain, with the most recent in 2012.
1 | Are vaccines available?
There is no vaccine for the Sudan strain of Ebola, which is responsible for the outbreak in Uganda.
Discussions are underway at the World Health Organization to determine which candidate vaccine could be deployed in a new clinical trial and potentially be licensed for use. But, with no vaccine currently proven to be effective, much of the standard medical response needs to be rethought.
The rVSV vaccine, manufactured by Merck, is licensed for the Zaire strain of the Ebola virus.
In epidemics linked to this strain, it can be used to limit the spread of the disease as part of a ‘belt’ vaccination strategy. This involves vaccinating people who have come into contact with sick people, people who have then come into contact with them, and caregivers of patients.
A second vaccine, manufactured by Johnson & Johnson, can be used during epidemics to protect people at risk of exposure to the virus. This might be a preventive measure for frontline workers before an epidemic has been declared, or for those living in areas not yet affected by the epidemic.
With the current Ebola outbreak in Uganda, all health organisations involved in the response will have to do without this vital tool until trials have been conducted and an effective vaccine has been found.
As with the clinical trials for the Johnson & Johnson Zaire strain vaccine, conducted in DRC in 2018-19, MSF is ready to assist in this research.
2 | How is the Sudan strain treated?
The previous clinical trials held in DRC identified treatments based on the use of antibodies, which are specific to virus strains: Mab114 and regn-eb3. These treatments significantly improve a patient’s chances of survival.
However, these antibodies are not effective against the Sudan strain of the disease.
So, treatment will involve managing the symptoms of the disease and providing specialised intensive care – including compensating for fluid loss, supplying oxygen and monitoring a patient’s blood and heart.
As in all Ebola epidemics, protective measures and infection control within healthcare centres are extremely important.
"The protection of frontline health workers is a major concern for MSF,” says Dr Guyguy Manangama, MSF’s deputy head of emergency programmes.
“We need to protect health workers to ensure the continuity of the health system by training them in infection prevention and control standards and by providing them with protective equipment."
Since the outbreak was declared, the Ugandan authorities have already confirmed the deaths of two health workers, a doctor and a midwife.
3 | What Ebola facilities does Uganda have?
During an Ebola outbreak, the medical response must take place close to communities in need.
"We know that the earlier patients receive medical attention, the greater their chance of survival,” says Guyguy.
“As the initial symptoms of Ebola are not distinctive, being similar to those of malaria or other viruses such as typhoid, the main issue is rapid access to information, diagnosis and care.
“In Ebola outbreaks, too many people still arrive at health centres with advanced disease or even die at home, infecting others in the process. This is what we need to avoid."
In past outbreaks, patients were also often taken straight to large facilities outside their communities. In many instances, this led to rumours circulating, hostility towards health workers and the rejection of the humanitarian response.
For these reasons, MSF recommends establishing small centres or isolation units where patients can receive first aid as close as possible to where they live. Meanwhile, larger referral centres can provide a wider range of care for patients in the advanced stages of the disease.
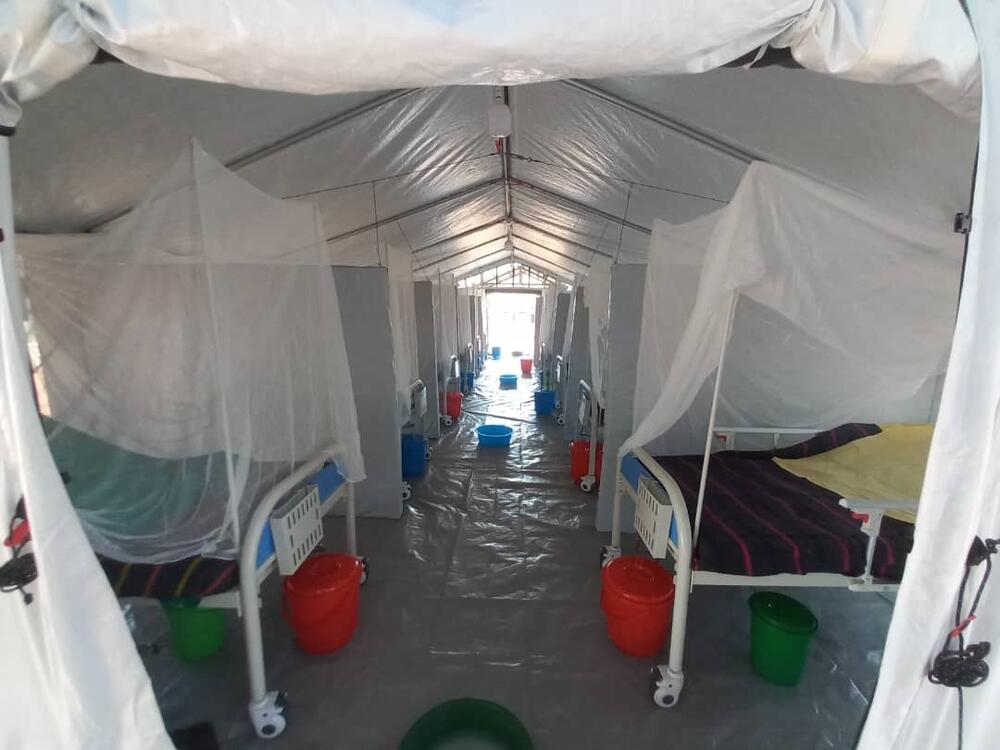
In Uganda, MSF is setting up small centres in communities such as Madudu (the epicentre of the outbreak) and then a larger 36-bed isolation unit with intensive care facilities in the district capital Mubende, 12 miles away.
MSF teams also plan to work with hospitals to create referral centres for healthcare workers infected by the disease.
4 | How far has this outbreak spread?
To bring an Ebola outbreak under control, it is essential to be able to rapidly detect infected people and identify their contacts, some of whom may have travelled far from the outbreak.
In Uganda, cases have been confirmed in five districts of the country, so patients and contacts will need to be identified and followed up across a relatively large area.
But, although the outbreak was officially declared on 20 September, several suspected deaths potentially linked to the disease were recorded as early as August. As is often the case at the beginning of an Ebola outbreak, tracking lags behind the spread of the virus. It is vital to reconstruct the early stages of the epidemic as accurately as possible to screen people for the disease and provide medical care in the right locations.
People must also be given knowledge and understanding of Ebola and be actively involved in the response. Community-based surveillance and contact tracing are needed to rapidly identify potential cases. Then, they and their families need to access appropriate healthcare or isolate themselves for 21 days.
To support this, social and economic barriers – such as the cost of transport to health centres, or costs linked to not being able to go out to work – need to be removed. This can be done by helping with transport, distributing food or kits to people self-isolating at home and offering psychological support to patients and their families.
Digital tools can also help with real-time monitoring of the epidemic. During the 2018-20 outbreak in DRC, Epicentre (MSF's epidemiological wing) developed new platforms to coordinate activities, systematically monitor and collect patient data track the evolution of the epidemic.
MSF is ready to make these tools available to the Ugandan health authorities.
MSF and Ebola
Ebola is one of the world’s deadliest diseases.
It is a highly infectious virus that can kill up to 90 percent of the people who catch it, causing terror among affected communities.
Ebola is so infectious that patients need to be treated in isolation by staff wearing strict protective equipment and clothing.