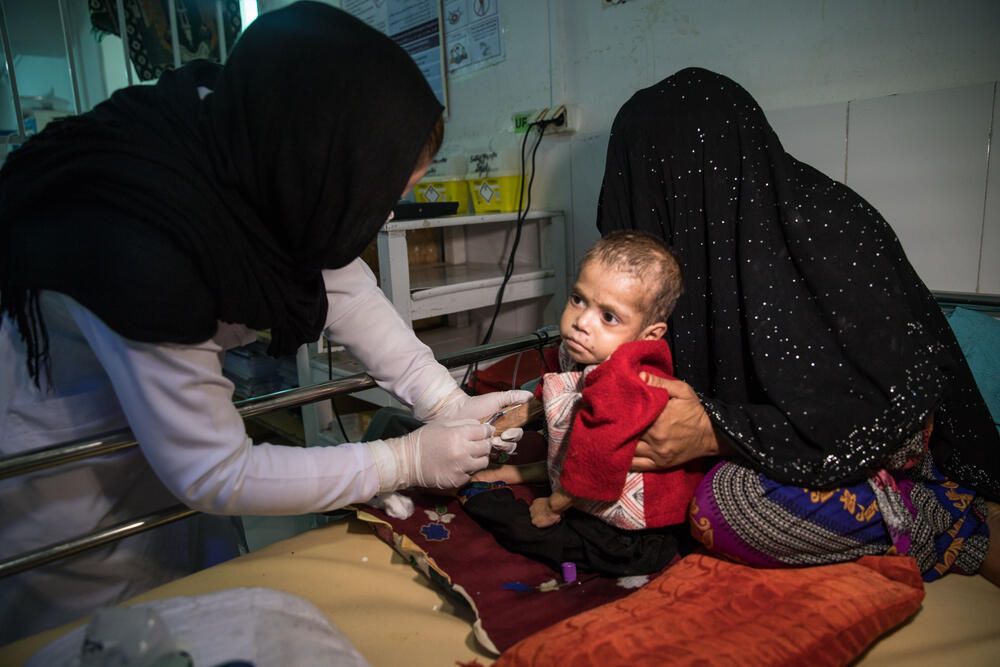
Asadullah Amini reports from Boost Hospital – one of MSF’s busiest projects worldwide – where our teams face a stark situation: a dangerous disease outbreak threatening a ward of sick children.
One child with the highly-contagious measles virus can infect 20 others.
But what happens when that child is already sick – severely malnourished, being treated in a busy hospital unit, surrounded by other vulnerable children?
The situation becomes critical.
Running out of beds
Right now, our feeding centre here at Boost Hospital in Lashkar Gah is very crowded.
Today, there are 50 patients, when this time last year we had only 15. We’re running out of space for new admissions, but more are still arriving.
“There are 306 patients admitted across the hospital right now, and almost 60 percent of them are paediatric cases. There are a lot of sick children here.”
Yesterday alone, 28 malnourished children were brought to our emergency room. We admitted the eight most critical – diagnosed with ‘severe acute malnutrition’ – and referred the others who were in a more stable condition to a facility run by another organisation.
We provide intensive treatment, and the children are with us for a minimum of five days. However, many have several conditions – perhaps diarrhoea, pneumonia, anaemia, or another medical problem. They may have already been in hospital for a while before they come to us, or we may refer them onwards once we have stabilised them. Some are so unwell they will need care for a long time.
There are 306 patients admitted across the hospital right now, and almost 60 percent of them are paediatric cases. There are a lot of sick children here.
The measles problem
There is another thing that complicates the malnutrition crisis: In just one week in March, Boost Hospital admitted 30 measles patients.
If a malnourished child arrives at the feeding centre with measles, we have to immediately admit them to a special isolation ward. We have to treat them for the virus and make sure they don’t infect the other children. We keep them there for about four days and follow protocols to tackle both conditions at the same time.
What makes it worse is that malnutrition makes children much more vulnerable to measles in the first place.
Just one child with measles is a risk. But, because of the way symptoms appear, we might not immediately know they have measles. This makes everything more challenging.
Parents might have travelled from far away to bring their child to the emergency room. The child doesn’t have any measles symptoms and they are in a severely malnourished condition, so we admit them to the feeding centre.
Then – and this happens very often – the next day a rash might appear, or they get a fever. The situation then becomes critical and we have to move them directly to isolation as a suspected case. But it could already be too late. The day after, there could be five more children in the same room all with measles symptoms.
The doctors and nurses have to always be alert and immediately identify the signs. Then we have to clean the beds, the equipment, and anything that the child might have come into contact with.
We go through this every time we find a case. It’s a lot of extra work for a team already under pressure, and we’re sending several children to isolation every week.
The economics of a crisis
During the change of government last summer, and for years before, fighting and insecurity prevented people from travelling to hospitals. There were often checkpoints and dangers on the roads. Now, travel is safer and people are coming in large numbers to our hospital. Many in serious conditions.
But this isn’t the only reason we are seeing more patients than before. It’s also about Afghanistan’s very serious economic crisis.
“For us, it doesn’t matter which government is in charge, what the security situation is… we are only thinking of our patients.”
There are a lot of jobless people or people who are not receiving their salaries, and the prices in the markets are so high because of inflation. This means that many people don’t have money to feed their families and cannot afford the things they need. There are also no fully-functioning health facilities in parts of our province other than what NGOs can provide.
The people are lost. They don’t know what to do and they don’t know what will happen next. I only feel certain about life, myself, when I am working at the hospital.
All this means that children are becoming sick. Parents are then coming to us – because we provide free medical care – from across this part of the country. It might be a six or seven-hour drive to reach us from parts of Helmand province. It’s very far.
At the same time, there is almost no primary healthcare left in Afghanistan – the basic services that could stop people from having to come to hospital in the first place. There is little vaccination coverage in villages across the districts and it’s hard to catch malnutrition early.
So, when they get here, the parents are just thankful if we can admit their child and do our best to protect them.
Proud to be MSF
I have been with MSF since 2010, not long after MSF began supporting Boost hospital. Today, it’s one of our biggest and busiest projects worldwide.
In just 24-hours we will see 1,000 patients in our emergency room and deliver around 60 babies in the maternity. I am still very, very proud of what we do.
For us, it doesn’t matter which government is in charge, what the security situation is… we are only thinking of our patients. We are proud of what we do, and it’s appreciated by the local people. They respect us and they trust us to provide high-quality care.
But, the truth is that we cannot do it alone. We can’t admit 500 patients to 300 beds, although we have recently increased our capacity to deal with the high number of admissions.
Other humanitarian organisations, governments and donors need to help us improve primary healthcare close to the villages and in the districts so people are not forced to travel for hours to reach care. Vaccination in particular is very important.
When people can access better care closer to home, we can help the sickest and most critical patients here.