South Sudan: “She arrived in one of the most critical conditions of pregnancy”
From the epicentre of South Sudan’s catastrophic flooding crisis, midwife Erin Lever shares the story of a critically ill mother and an unbelievable journey to reach care.
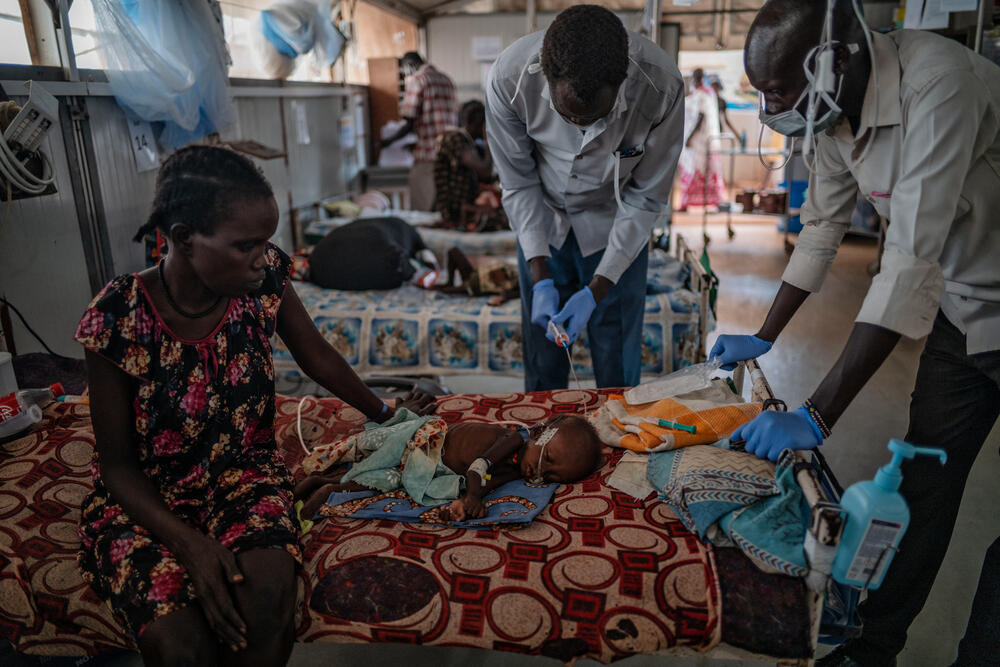
For the past six months, I have been working for Médecins Sans Frontières / Doctors Without Borders (MSF) in a camp for displaced people in Bentiu, South Sudan. The MSF hospital here is the only secondary healthcare facility serving the camp's 130,000 residents.
In the maternity department, we see women who are experiencing complications in their pregnancies, and often emergency referrals that arrive at the last minute in very critical conditions.
"These men have walked for three hours, through the floodwater in the middle of the night, carrying the pregnant woman on a blanket"
As a midwife, I am always on-call on the radio to assist the team with any complicated cases. One night, I receive a call that a woman in the final weeks of her pregnancy has arrived with significant bleeding.
This is a medical emergency.
The long journey
It's dark, and when I walk into our maternity unit, our waiting area outside is unusually crowded. There are at least ten men. One of my colleagues tells us that they are the family members of the woman and that when her condition became serious, they set off, on foot, to carry her to the hospital.
This year’s floods are the worst that South Sudan has witnessed for the past 60 years. They have almost surrounded the camp here and many villages are cut off from everything, including food and healthcare.
These men have walked for three hours, through the floodwater in the middle of the night, carrying the pregnant woman on a blanket. They explain to my South Sudanese colleagues that in the deepest of water, the taller men took their turn carrying, and the shorter men took over in the shallower stretches.
They are sodden and muddy and look exhausted. The whole team, including midwives who have had incredibly challenging lives themselves, are amazed at their resilience.
Critical condition
Quickly, we assess the woman. She is slightly anaemic from the blood loss but is otherwise stable, although still bleeding. Her baby, thankfully, is still alive.
We suspect a partial placental abruption – where the placenta starts to separate from the uterine wall before delivery – one of the most critical conditions in pregnancy. It can cause a life-threatening haemorrhage for the mother, and because the flow of blood to the placenta is compromised, the baby can pass away.
We have a small blood storage unit here where we collect donations from volunteers living in the camp. We are one of the only maternity facilities in the area fortunate enough to have this option.
However, blood is often a challenge to come by, particularly for rarer blood groups. Luckily this woman’s blood group is a common one, which means we are better prepared if she does need a transfusion.

Help us prepare for the next emergency
Two emergencies
During the assessment, we find that the woman is already in the early stages of labour. We get her consent to accelerate the process so that the bleeding stops and the baby has a better chance of survival.
She has already had several pregnancies, and so her labour progresses quickly. Soon her baby is born… but not breathing. We start resuscitation.
This is what we feared – it is likely due to the placenta only partially functioning during labour. At last, there’s a cry and a wave of relief breaks over me. The baby girl is breathing on her own.
She will be fine.
“The blood loss is rapid and the woman is showing signs of her body not coping well. She starts to lose consciousness.”
But there’s no time to relax: the mother has a heavy postpartum haemorrhage.
We start our emergency haemorrhage protocol and it becomes clear that the woman’s condition is unstable and that she will need a blood transfusion. The blood loss is rapid and the woman is showing signs of her body not coping well. She starts to lose consciousness.
It is the middle of the night and we don’t have enough staff to deal with the two emergencies simultaneously. However, members of our nearby neonatal nursing team step in to help us.
Stepping up
Because blood stocks are hard to come by, we can always get one unit of emergency blood from our bank, but after that, the patient’s wellbeing often relies on donations from family members. This can sometimes be difficult as people tend to donate blood only in emergencies.
However, on this occasion, the woman’s relatives step up without hesitation.
Many of the men who carried this patient here are very young adults. Their thin bodies show the consequences of the harshest living conditions. It is touching to see them, having been through an immense physical feat to arrive here, now lining up to donate a pint of blood to help us save their relative.
By early in the morning, the woman has received three units of blood and it is clear now that she will be okay.
The night shift team go home; alongside this emergency, they have also been attending to the other women in the maternity ward. We are all exhausted and feeling the after-effects of our adrenaline-fuelled night.
Years of instability means that South Sudan has a very limited and unreliable public healthcare system – in this region, MSF provides much needed, high-quality care. But the floods are impacting all aspects of people’s lives, cutting them off, increasing the risk of disease outbreaks like cholera and malaria, while also making it even harder for people to access basic services.
Without the MSF hospital and teamwork from the maternity and neonatal staff, the strength and determination of her family, and the woman's own endurance, this patient and her baby would not have survived.
MSF and the South Sudan flooding crisis
South Sudan is facing a severe flooding crisis that has hit almost 800,000 people. Vast regions of the country are affected by rising water levels. Tens of thousands of people have been forced from their homes and deadly disease outbreaks are on the rise.
Since May 2021, flooding has hit eight out of 10 states, with Jonglei and Unity states – where MSF runs three medical projects – being the worst affected.