Yemen: How conflict and poverty combine against mothers and children
When Um Ayman began to have pain in her stomach, she didn't think it was the start of going into labour. She wasn’t nine months into her pregnancy yet.
She went to the pharmacy, whose volunteer “doctor” was the only option for medical advice in her village, Al-Malahaet – an isolated place near to both the Saudi border and the frontline, where Saudi and Yemeni troops face off against fighters from Ansar Allah.
“The doctor told me that it was not time for me to give birth and gave me some intravenous fluids,” says Um Ayman.
“But then my waters broke.”
“We are in what might be called a healthcare desert here”
Um Ayman spent an agonising three days at home trying to give birth before her family managed to scrabble together the money for the five-hour car ride to Haydan.
There, staff at the Médecins Sans Frontières / Doctors Without Borders (MSF) hospital found that her baby had been lying horizontally across her uterus, instead of straight down. The baby had died during labour and Um Ayman needed urgent surgery to remove her unborn child and save her own life.
Rising numbers
Stories like Um Ayman’s are all too common in Haydan, a town of traditional brown houses, lush khat fields and the ruins of buildings bombed by Saudi jets.
While the town is no longer attacked like it was in the first years of the war – houses, the girls’ school and even the MSF hospital were all destroyed – explosions from airstrikes still echo in the surrounding hills.
The area’s remoteness and inaccessibility combine with active conflict, poverty, and a barely functional healthcare system to mean that few people have access to the medical care they need.
The hospital, rebuilt and reopened by MSF in 2017, is one of the very few options.
“We are in what might be called a healthcare desert here,” says David Charo Kahindi, MSF’s project coordinator in Haydan.
“There are very few health facilities and things seem to be getting worse. Our paediatric admissions have increased by 45 percent and the number of deliveries by 30 percent compared to the same period last year.
“Overall, we are seeing more serious patients coming to us: while the number of people coming to the ER is stable, we are admitting double the number of them than we were last year.”
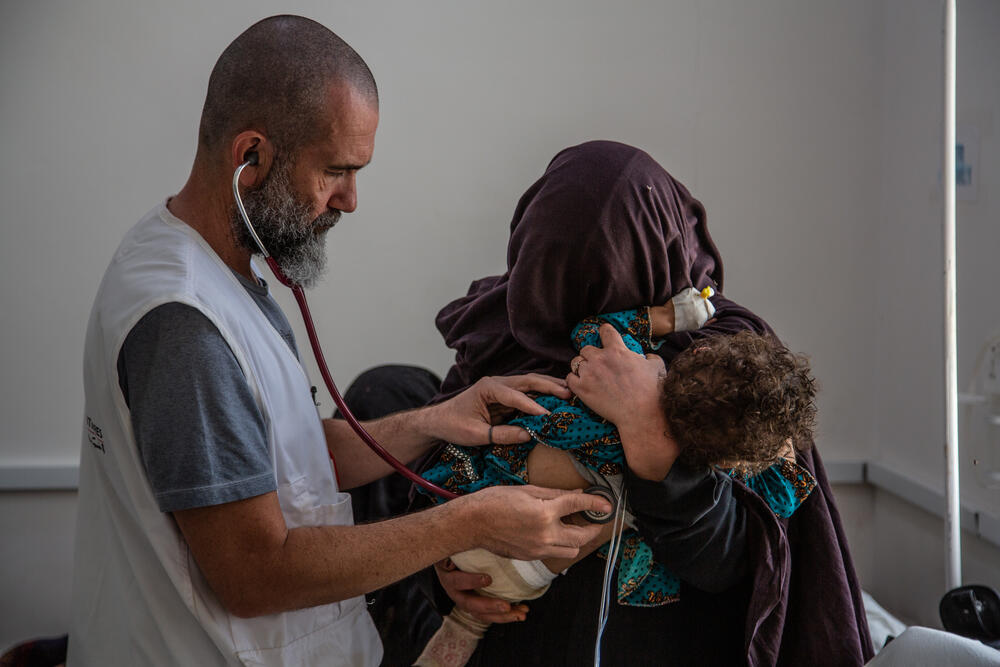
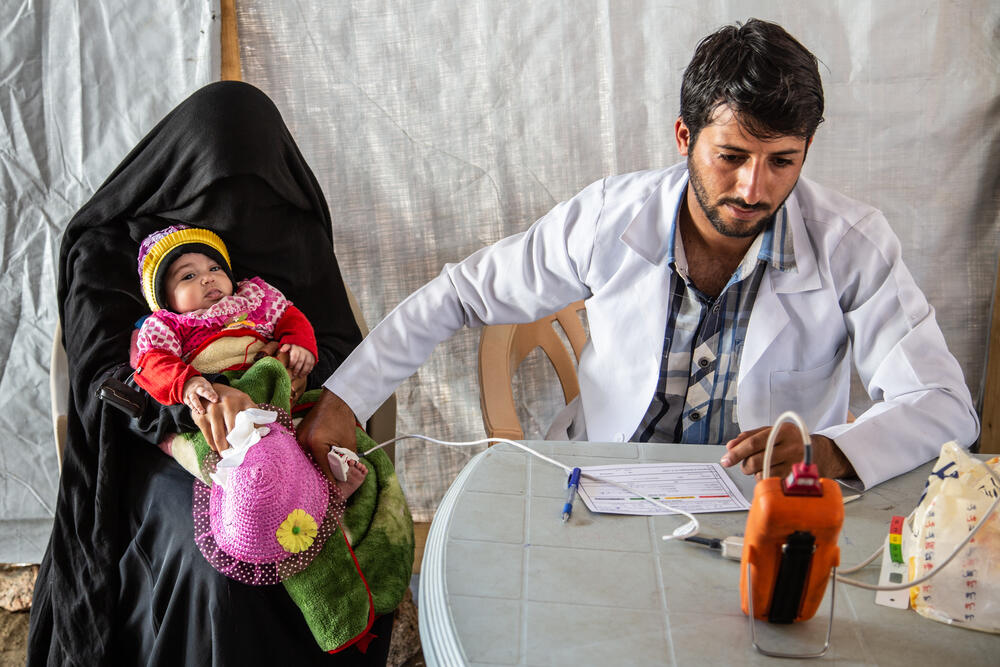
Mothers and children
The hospital treats relatively few people wounded by the fighting itself, at around 15 a month. Instead, much of the activity focuses on the needs of mothers and their children.
On average this year, the team have assisted 176 deliveries and admitted 92 children to the wards every month.
The children were mostly sick because of respiratory tract infections and diarrhoea, diseases often associated with poor living conditions.
Only 40 percent of the mothers who give birth in the hospital have been able to access antenatal care. This means many complications go undetected until a mother goes into labour, just like Um Ayman.
Medical care where it's needed most
Help us care for people caught in the world's worst healthcare crises.

“At the end of last year, we opened an operating theatre in the hospital so that we would not have to refer people to Sa’ada City,” explains Kahindi.
“People here already have to travel for many hours to get to Haydan, so now it is better that we can offer care for women who need caesarean sections or people who need other types of general surgery, without them having to travel even further.”
The cost of reaching care
Travel has become harder in recent years as the price of fuel has increased and inflation has reduced people’s purchasing power.
“We live in Lower Duweib and it takes six hours to get here to Haydan,” says Hamid Ali, 33, who had accompanied his uncle to hospital after he broke his leg in a car crash.
“The local health centre has one worker only and they can only do small dressings, so we had to pay 100,000 YER (£289) to get a car to bring us here.”
These are astronomical sums for families in a region where most people are farmers and herders, living in an area heavily affected by conflict.
“We have livestock and we hear the fighting every day,” says Ali.
“Sometimes the shelling hits our village, but we do our best to live an ordinary life.”
Restrictions on aid
The conflict doesn’t only create urgent needs for people living in the area, it also makes it more complicated for humanitarian organisations to respond to the crisis.
The different sets of authorities in Yemen all regulate the work and movements of humanitarian organisations to some extent, with some of the conditions put in place by Ansar Allah being particularly demanding.
Obtaining permission to work in places close to the frontline, such as Haydan, is often especially difficult due to the area's sensitivity. MSF is the only humanitarian organisation with a permanent presence in the district.
“We see that there are huge needs here, and while we have already started new services and are expanding the hospital further, we cannot meet all the needs alone,” says Kahindi.
“In order to meet the existing needs and prevent the situation from deteriorating further we need other organisations to commit to providing services here – and for the authorities to facilitate their access.”
Um Ayman is overcoming the trauma of her experience. Despite the fear she feels, she is getting ready to go back into the operating theatre and have her wound cleaned.
“I am scared,” she says.
“I don’t want to die without seeing my children again.”
What had been a relatively normal complication has become an ordeal that nearly killed her and has now left her traumatised.
“Without better access for humanitarian organisations in the area, more people like Um Ayman will suffer – and some even die – from medical issues that are preventable and treatable,” adds Kahindi.
“That cannot be allowed to happen.”
Support MSF in Yemen
The increasingly brutal conflict in Yemen is leading more women to die from childbirth complications and a devastating number of children aren’t making it to their first birthday. Healthcare is severely limited across the country.
Médecins Sans Frontières/Doctors Without Borders (MSF) provides life-saving medical care in hospitals across Yemen.