The ward that should not exist: Battling measles in Bangladesh
In a pink room decorated with white flowers at Médecins Sans Frontières’ (MSF) Kutupalong field hospital in Bangladesh, a woman lies curled around her sleeping child.
Next to her, a young mother cradles a baby, whilst her other daughter plays with a balloon.
Rows of beds stretch in either direction, mothers and children sitting or lying quietly in every one. It could be a peaceful scene, except for the intravenous lines snaking up from each child’s arm to a saline drip.
None of these children should be here
This is an isolation ward and all these children are critically ill with measles. Many have additional complications, such as pneumonia and malnutrition. The nurse checks vital signs every hour.
For a ward full of young children, it is eerily silent – most of them are semi-conscious.
“Since November the cases have been increasing and increasing. Now it’s overflowing”
None of these children should be here. Measles is a preventable disease; a simple and safe vaccination protects against the illness.
With routine immunisation, these children should not have caught the virus.
Overflowing with patients
Neither should this ward exist. It is usually an intensive feeding unit for severely malnourished children. But four weeks ago, to cope with the growing number of critical measles cases needing inpatient intensive care, staff had to transform it into an emergency isolation ward.
In the first four weeks of the year, MSF saw a 40 percent jump in measles cases treated in our facilities in the refugee camps.
In January alone, around 120 patients were admitted to MSF isolation wards, with more than 900 people treated as outpatients.
“Since November the cases have been increasing and increasing,” explains Mohammad Younus Ali, an MSF nurse in the Kutupalong Hospital. “Now it’s overflowing”.
Children at risk
A highly contagious airborne virus, measles is particularly dangerous for children, putting them at risk for severe pneumonia, encephalitis (swelling of the brain) and death.
Over 80 per cent of MSF’s current measles patients are under the age of five. Thirteen have died from measles in MSF clinics since the outbreak started.
Nurata’s nine-month-old daughter Nur Salima first developed a fever six days ago, and received treatment in Kutupalong hospital. Nurse Younus explains that baby Nur Salima was barely conscious when she arrived in the emergency room. “I saw [Nurata’s] face at the day of admission; there was lots of fear in her face.”
“It’s like suffocating”
The doctors gave her daughter oxygen to help her breathe, and antibiotics to fight secondary infections.
Severe respiratory infections and difficulties breathing are common complications with critical measles cases. MSF doctor Nowshad Alam Kanan describes how young children arrive at the clinic, gasping for breath. “It’s just like suffocating,” he says.

Get closer to the Frontline
Get the latest news, stories and updates, straight to your inbox.
Tell-tale rash
Seven kilometres away, in the southern part of the refugee camp, MSF is receiving patients in Jamtoli primary health centre.
Like others, this clinic is also overwhelmed. As a primary health centre the isolation ward has five beds, which is normally sufficient – except now the clinic has been receiving ten to fifteen patients daily, according to Dr Nowshad.
In Jamtoli’s isolation ward, Romida and her husband Abu Sufian watch over their ten-month-old son Forkan.
The couple got married in the refugee camp, and Forkan is their first child. His face is covered with the tell-tale red measles rash, his eyes swollen and gummed shut.
Listless and in pain, he writhes on his mother’s lap as she rocks him gently. Concern is etched on the young parents’ faces.
3,930
BIRTHS ASSISTED BY MSF IN BANGLADESH IN 2024
624,100
OUTPATIENT CONSULTATIONS IN BANGLADESH IN 2024
3,330
PEOPLE TREATED FOR INTENTIONAL PHYSICAL VIOLENCE IN 2024
No access to vaccination
When her son became sick, Romida was so scared she stopped eating. Suffering from a high fever, diarrhoea and experiencing difficulty breathing, Forkan had also refused to drink.
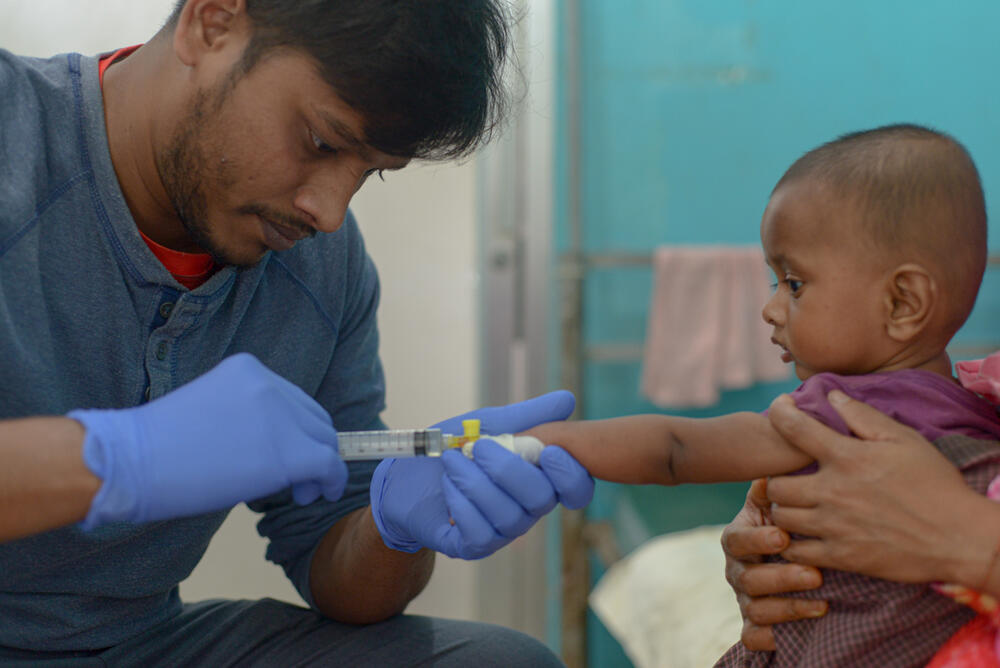
Now, a nurse hands Romida a syringe filled with an oral rehydration solution, which she gently tries to drip into her son’s mouth.
Measles can cause oral infections, which makes eating and drinking exceptionally painful.
Despite her encouragement, little Forkan will not drink.
The Rohingya have suffered decades of persecution and restrictions on healthcare in Myanmar; as a result, most people never received routine immunisation for infectious diseases.
The lack of quality routine immunisation for Rohingya refugees in the camps means that babies like Forkan who are born here are at risk of catching preventable infectious diseases like measles.
Indescribable joy
After five days in the isolation ward, Nurata’s daughter Nur Salima improved and was finally strong enough to be discharged. Having nursed her back to health, Nurse Younus is delighted.
The feeling of watching a patient survive “is indescribable” he says, overjoyed.
Forkan, however, is still fighting. Unable to drink any fluids, he was transferred to MSF’s Goyalmara hospital for intensive care.
MSF’s team will do everything they can to save his life.
MSF in Bangladesh
Hundreds of thousands of Rohingya have sought refuge in Bangladesh but now live in a precarious situation.
Médecins Sans Frontières/Doctors Without Borders (MSF) has worked in Bangladesh since 1985 and in 2017 we rapidly scaled up our operations in Cox’s Bazar in response to a massive influx of refugees after a renewed wave of targeted violence by the Myanmar military.
In the overcrowded settlements where most Rohingya live, water and sanitation activities are an important part of our efforts to stop the spread of disease. Our clinic in Cox's Bazar offers comprehensive basic and emergency healthcare to Rohingya refugees and the local community.
We also run inpatient and laboratory services. In Kamrangirchar, a slum area in Dhaka, the capital of Bangladesh, we provide services including reproductive healthcare and support for survivors of sexual violence.