Malnutrition: “It turns simple conditions into something deadly”
Malnutrition is more than just hunger. And it’s really complicated to treat. It requires specialist medical care, specialist knowledge, and a lot of support.
My name's Marc Woodman. I’m a medical doctor in the NHS, focusing on what’s known as ‘internal medicine’. I usually work at a hospital in London looking after acutely sick patients.
I’m also a doctor with MSF. I’ve recently returned from South Sudan – where I was working at a huge displacement camp of around 130,000 people, near the town of Bentiu.
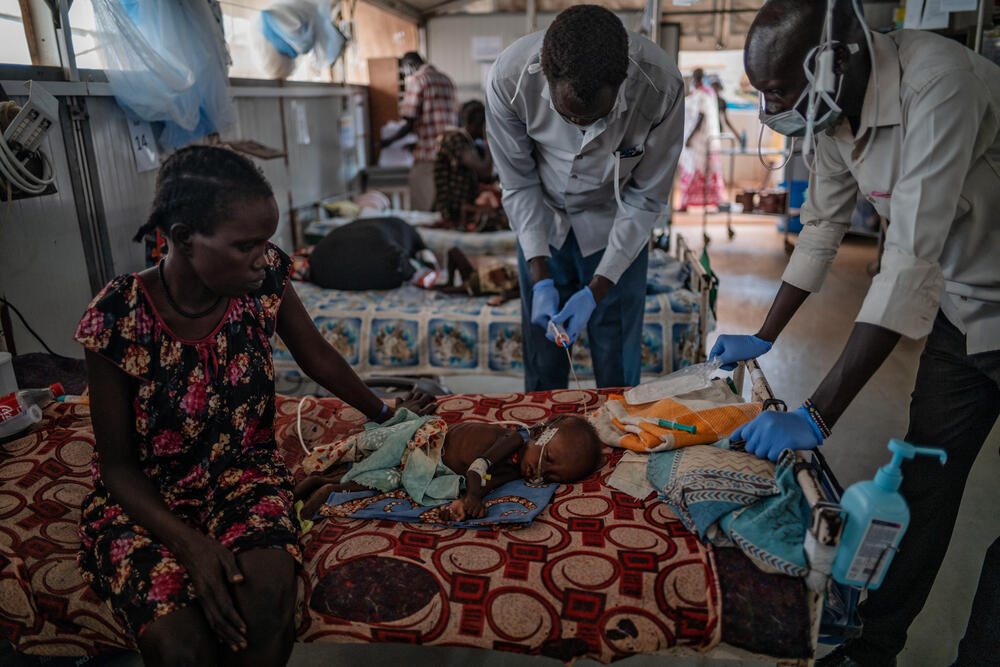
“When a child comes in with severe acute malnutrition, they look physically very different to any other child. It’s difficult to even assess them properly.”
I think Bentiu camp is probably one of the hardest places to live in the world. The camp was originally set up to protect civilians fleeing violence and instability. But recent crises, particularly catastrophic floods, have forced even more people to move there.
There’s a huge number of people packed into a relatively small space that’s very hot and completely surrounded by water. Sanitation is a challenge, leading to infections from waterborne diseases.
It’s a really difficult place to work, but an even more difficult place to live.
In the middle of this crisis, malnutrition is a huge issue that we see a lot of in the hospital.
More than hunger
Malnutrition is a chronic lack of access to nutrients, to carbohydrates, to all the things that your body needs to work. And, after a prolonged period without these things, your body can start to change.
Your metabolic rate slows and your body’s systems start to break down. Your immune system in particular is severely affected, becoming much, much weaker.
This means that when someone is severely malnourished they're at huge risk of infections and secondary complications. This can mean everything from malaria to pneumonia and diarrhoea, to all sorts of other conditions.
And, while a few groups are particularly vulnerable, the most important is children under five. Caring for them can be really complicated, really hard and very intensive.
When a child comes in with severe acute malnutrition, they look physically very different to any other child. It’s difficult to even assess them properly – for example for dehydration – because of the changes to their skin and the distribution of fat in their body.
Most worryingly of all, feeding them can be dangerous, even fatal, because their bodies have changed so dramatically.

New nutrients and fluids can quickly change their balance of electrolytes and make them really, really sick. This is sometimes known as refeeding syndrome.
Our team has to use special foods which need to be controlled quite precisely, and we monitor the children until they’re out of the woods.
As you can imagine, it's a very challenging thing to do in an environment without many resources.
A mother and a bundle
This is one of those stories that I really hold onto…
A mother and her baby had been referred to our hospital, partly because she couldn’t produce any breastmilk. In fact, she was incredibly unwell – she’d clearly been sick for a really long time and was very malnourished and underweight.
She had a new diagnosis of HIV that was severely affecting her, and, from her symptoms, potentially tuberculosis (TB) as well. I have a lot of experience with HIV and this woman had one of the lowest levels of immunity I have ever seen.
I usually work as a doctor for adults, so I concentrated on getting her immediately started on treatment. But, while we were working I thought “Well, she’s got this baby… but where is it?” I couldn’t see a child anywhere in the room.
That’s when the grandmother pointed to a tiny blanket on the bed. Just a little, tiny bundle.
Peeling it apart, there was this very small and really sick-looking baby. We quickly checked him and he only weighed 1.8 kg. In the UK, a normal birth weight is about 3.5 kg, but this little boy was already 40 days old. I called my colleagues in paediatrics who immediately swept this little one off to their ward.
They managed to start tube feeding him, and his wonderful grandmother stayed to help look after him. I later found out from that team just how unwell the little boy was – on the brink of passing away if he hadn’t got treatment there and then.
I started popping by the ward towards the end of my shifts to see him and his grandmother. She always greeted me with a huge smile.
Within 10 days, the little boy was putting on weight well. We’d also started him on treatment for HIV. Unfortunately, his mother was still really poorly. We admitted her to our TB ward.
Eventually, she started putting on weight too, and the HIV and TB treatments took effect. After almost three months, she was finally well enough to go home and be with her little boy.
Critical care
Malnutrition and infection go together. In South Sudan, it means that medical conditions that we might expect to recover from in the UK can turn deadly.
The people in Bentiu camp have already been through horrendous things and have very limited access to help of any kind. If MSF wasn’t there, there would be no other option for medical care.
It would turn an incredibly challenging place to live into a completely impossible place.
The MSF Malnutrition Appeal
Malnutrition is about more than hunger. It’s about healthcare.
Children with severe malnutrition struggle to fight off deadly diseases such as malaria, pneumonia or measles. Even giving food itself can bring on dangerous medical complications. That’s why MSF teams are delivering expert care to save young lives.