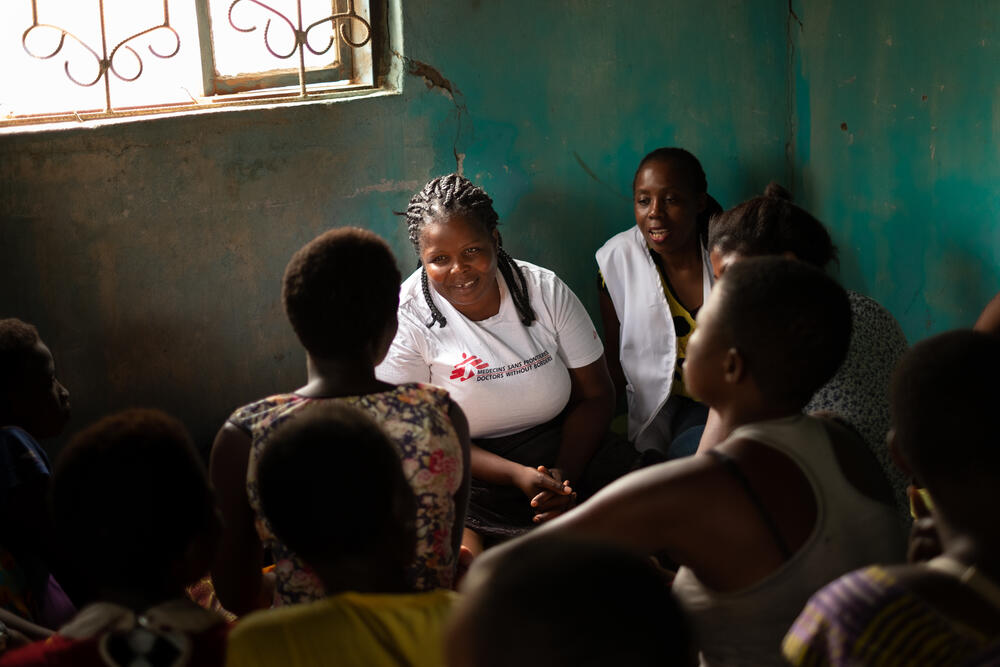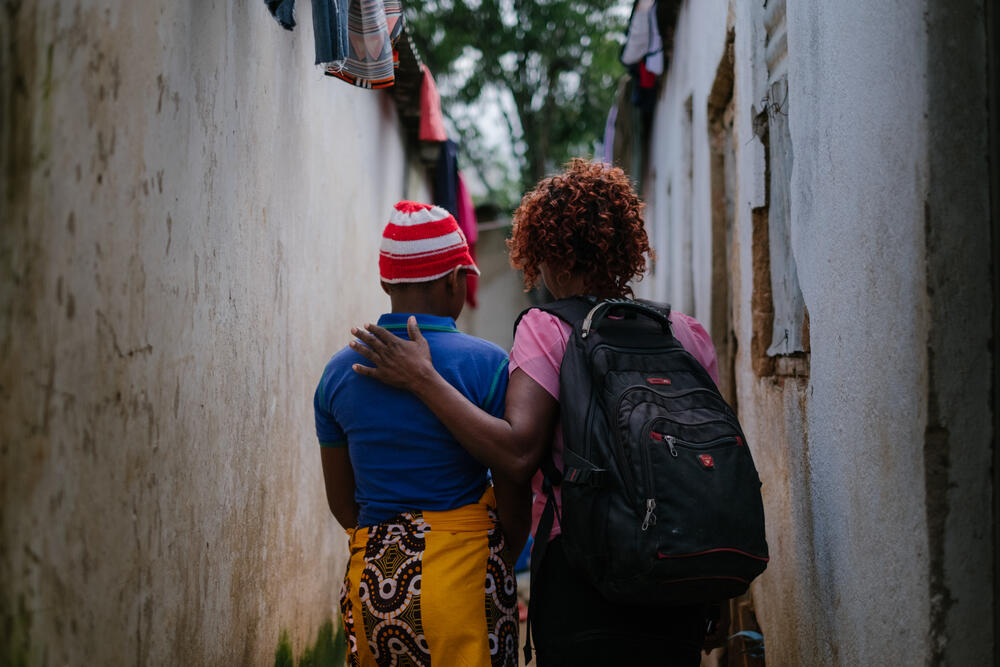Malawi: The sex workers helping others fight HIV
In southern Malawi, an MSF project is helping thousands of women who earn their living from sex work to overcome barriers in accessing healthcare – partly by training and employing some as community health workers.
*Names have been changed unless otherwise indicated
Bernadette lost both parents when she was seven-years-old.
She was taken in by her grandparents, who would have to send her to school without food.
“I started having sex in exchange for things as my grandparents were not able to provide me. This is how I got pregnant and dropped out of school,” says Bernadette who moved from her village to Dedza, Malawi at the end of 2018.
“When I became a sex worker I didn’t know anything about condoms, or any other family planning methods. I had heard of HIV but never thought about contracting it myself.
“This was the very first time I was given information on issues like HIV testing and sexual health,” says Bernadette, after Emily – an MSF community health worker – gave her a health education session at the bar where Bernadette lives and works.
“I saw it as an amazing opportunity that could help me to be healthy, no matter my circumstances.”
Learn more about HIV/AIDS
We pioneered treatment in Africa and have helped millions of people globally
Emily listened closely to what she had to say, because she too was a sex worker. She knew where Bernadette came from and what she was facing every day.
If we are to deal with HIV once and for all, the first step is to accept and recognise that, despite being different, we are all human beings
Stigma and violence
In Malawi, where poverty and unemployment remain high, many women like Bernadette turn to sex work – offering sexual services in exchange for payment of some sort – to support themselves and their families.
However, Malawi has one of the world’s highest rates of HIV, and while the country has made huge strides in fighting the epidemic, sex workers remain extremely exposed.
With much lower access to health information and healthcare than the general population, sex workers are over five times more likely to contract HIV and face much higher risks of unwanted pregnancy and sexually transmitted infections (STIs).
Sex workers report stigmatising attitudes and often violence in their daily lives – from police, clients, bar owners and even partners. While these risks are seen by many as part of the job, empowering sex workers with knowledge and prevention methods is key to protecting their health.
“In the past, most sex workers shied away from visiting health centres for fear of discrimination and stigma, especially if they were found HIV positive,” said Alice Matambo (real name), an MSF community health worker in Dedza.
“If women needed post-exposure prophylaxis (PEP) – a treatment that prevents HIV if taken within 72 hours of exposure – they just didn’t go to the hospital because they knew they wouldn’t be helped.
“Sex workers need healthcare in their daily lives: if a condom bursts, if they have an STI, or need to be screened for cervical cancer.”
Understanding the challenges
Recognising these gaps, MSF has been working with the Ministry of Health to provide services that meet the specific needs of sex workers.
To connect with sex workers in the towns of Dedza, Mwanza, Zalewa and Nsanje, MSF has trained sex workers like Emily and Alice as community health workers – as they have themselves experienced the challenges and dangers associated with sex work.
This shared experience enables them to discreetly link with other sex workers, understand their health situation and explain the medical services they need. Medical staff in the project have also been given sensitivity training to provide friendly services for sex workers.
“We approach sex workers gently and with respect, which makes them accept our approach, and look for medical help,” Emily says.
Margaret, an MSF community health worker in Mwanza, explains this way of working:
“My job includes going door to door and visiting bottle stores and brothels where I meet sex workers and provide them with information related to HIV testing and how they can take care of their health.
“For those who agree to be tested for HIV we set up a home visit.”
One-stop clinics
The community health workers also guide sex workers towards “one-stop” clinics run by MSF within Ministry of Health facilities or in rented rooms in communities close to where sex workers live and work.
The “one-stop” clinics are easy for sex workers to access discreetly and at convenient times.
In a single visit, staff provide services like HIV testing, treatment and counselling; TB screening and referral for care; and sexual and reproductive health care – including screening and treatment for STIs, access to contraception choices, cervical cancer screening, and treatment for sexual violence, which is either delivered on the spot or through referral.
“With these services, I feel more empowered than before and I am able to negotiate protection with my clients. I know how to put a condom on properly and we now have lubricant which prevents accidents,” says Bernadette.
A positive impact
Many of the community health workers employed by MSF say they resorted to sex work after having children at a young age and being abandoned by their families or losing the support of their husbands to take care of their children.
They are often shunned by their families and communities, facing abuse and hostility because of what they do.
The presence of the project has seen reduced levels of stigma against sex workers, as well as a positive impact on their access to HIV testing and sexual health care.
“While some people used to look at us as animals, things have changed,” says Margaret.
“Today, the perception that people have towards sex workers is improved. Today, people understand that HIV affects everyone. And if we are to deal with HIV once and for all, the first step is to accept and recognise that, despite being different, we are all human beings.”
MSF in Malawi
Malawi is a landlocked country in southeast Africa. It has one of the highest prevalences of HIV in the world, with 9.2 percent of the adult population – one million – living with the virus in 2018.
Médecins Sans Frontières/Doctors Without Borders (MSF) is working to reduce HIV deaths in Malawi by facilitating earlier treatment and more advanced care. We have been in the country since 1986.
Over the years, our teams have provided a wide range of medical care and responded to natural disasters, including Cyclone Idai in March 2019.