Malaria: How Paul survived “the red bed”
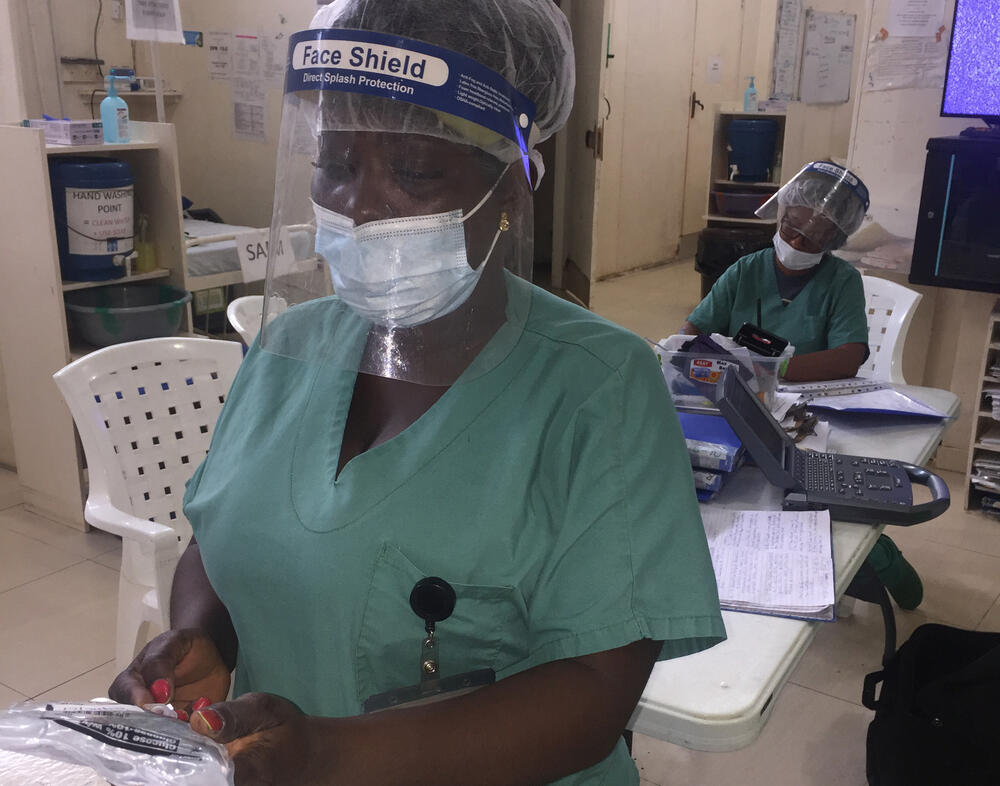
At the MSF Children’s Hospital in Monrovia, Liberia, critically ill patients are treated for the life-threatening complications of malaria – patients like Paul B. Morris Junior, who arrived unconscious.
Ten-year-old Paul B. Morris Junior had been unwell with malaria for a number of days.
His grandmother had taken him to a local hospital and he’d been prescribed medicine, but he continued to complain that he felt sick. Then he fell unconscious.
Paul’s grandmother rang his mother, Lydia, in distress. She raced home.
“I met him at the back of the house, lying down, you know, [his body] jerking”, she explains – a tell-tale sign that the malaria was not only severe but possibly already affecting his brain.
Cerebral malaria
Malaria, spread by the bite of a female Anopheles mosquito, is the number one cause of illness and death in the West African country of Liberia. Malaria occurs year-round, and people can suffer repeated attacks throughout their life.
If left untreated, or not treated properly, it can cause severe and life-threatening complications, especially in children. Cerebral malaria is one of the most dangerous.
Paul, who was normally so quick to laugh, and happy learning how to read and playing football, was now comatose. His future uncertain.
Lydia and her husband found an auto-rickshaw and eventually arrived at MSF Children’s Hospital (also known as Bardnesville Junction Hospital), run by Médecins Sans Frontières / Doctors Without Borders (MSF).
Opened in 2015, the hospital provides free healthcare, including surgery, for severely sick children and young infants in Liberia’s capital, Monrovia. In 2020 alone, the hospital admitted 4,251 patients.
The red bed
In the emergency department triage, Paul was seen by a nurse and nurse aide who took his vital signs, confirmed his critical state, and sent him through to “the red bed”.
The red bed in the emergency room is not just a bed. It’s surrounded by a range of emergency care machines, materials and medications that allow the medical staff to assess, treat and stabilise critical patients as efficiently, effectively and quickly as possible.
For the team caring for Paul, they inserted a tube to intravenously deliver diazepam and reduce his convulsions. They also carried out a rapid diagnostic test to confirm his case of malaria and identify his low levels of haemoglobin – the protein that carried oxygen through the blood – an indicator of anaemia.
Paul was also hooked up with a mask to receive oxygen therapy and immediately started on antimalarial and antibiotic medicines to treat the illness and his fever.
Only then, stabilised and with his treatment underway, could Paul be admitted to the intensive care unit (ICU).

Help us prepare for the next emergency
Team Paul
Roseline Biago, an ICU nurse at the MSF hospital, has worked alongside her team treating many patients with cerebral malaria. Typically, they arrive unconscious, convulsing, with a persistent high fever.
“Some of them will be talking off their head,” explains Roseline.
“Sometimes they will be hallucinating—the parents or carers will be concerned about what is happening.”
In Paul’s case, he became highly combative, fighting off the staff. For his mother Lydia, this was a particularly confronting sight.
“I began to cry,” she says.
“But later on when I saw the movement of the nurses, the doctor and the physician’s assistant (PA), I became relaxed.
“The whole team came over to him, started fighting to stabilise him, checking the blood pressure, checking his heart rate and things. I gained courage. I sat down and I just started looking at them: Roseline, Victoria, PA George.”
Nurse Victoria Pewee could see how worried Lydia was. But, for the medical team, parents and other carers can play an important part in providing good quality care.
So, Victoria encouraged Lydia to get involved in the treatment, telling her:
“Come and report anything abnormal you observe so that we can be able to take an intervention right away.
“Maybe if Paul has diarrhoea or a fever—though we are checking all the time—or if the child is vomiting, you will be able to tell us. Because you are there.”
Lydia’s hope and confidence were bolstered.
“Each time I asked a question they were willing to answer me, to make me understand,” she says.
Unresponsive
Still unconscious in the ICU, unresponsive to anything but intense stimuli such as a pinch of his fingertip, Paul’s intake was limited to intravenous fluids to avoid dehydration and low sugar levels as anything more could have destabilised his condition. His convulsions were becoming less worse.
As his level of consciousness improved, the paediatric consultant, Dr Tim Pont, advised Paul could now start feeding through a nasogastric tube that would deliver food directly to his stomach via his nose.
Malaria: Our work in numbers
249 MILLION
CASES OF MALARIA WORLDWIDE IN 2022
80%
OF MALARIA DEATHS IN AFRICA ARE CHILDREN UNDER 5
3,877,100
MALARIA CASES TREATED BY MSF IN 2024
However, a blood test revealed unwelcome news: Paul’s haemoglobin levels had dropped again, requiring an emergency blood transfusion from the hospital’s blood bank.
The neurological effects of malaria had also meant that Paul stayed combative for several days. Lydia recalls how he slapped a nurse aide and kicked a doctor.
So, she held him and talked to reassure him.
“Paul, don’t be afraid of these people. You are not well, that’s why I brought you here,” she said.
“These are the people who look after you, so you’ll be well. They are your friends.”
A dramatic turnaround
The most severe malaria patients in the hospital can take up to a week to regain consciousness. Only then may they be moved out of intensive care and to the general paediatric ward for the final stage of their recovery.
By Paul’s fourth day in the ICU, the anticonvulsants had worked and he was now calm. As his consciousness returned, Paul began to respond to people’s voices.
Nurse Victoria describes how they coaxed Paul to talk:
“Little by little I said ‘Paul, say yes... do you wanna eat?’, and he’d say ‘Mmmm!’. And I'd say, ‘No, say yes properly’ because we were trying to see how well he was oriented.
“And little by little, he could talk, he became alert, he wanted to eat and could tell us that he wanted to eat.”
George Tengbeh, the PA on Paul’s medical team, has one word for Paul’s recovery:
“It was dramatic! Seeing a child that is almost unconscious… from there he became conscious, became alert and started communicating. Initially, his communications were incorrect but later they started becoming correct sentences and making sense.”
The team was elated.
“I sat right beside him,” says Lydia. “I told them, ‘I’m not leaving from his side’. He did well.”
Incredibly, just four days after being discharged, Paul sat his school exams in English and Maths.
Prevention is better than cure
For the team at the MSF Children’s Hospital, the young patients that are suffering complications of severe malaria are a constant reminder of the importance of prevention and early diagnosis.
Insecticide-treated bed nets are one of the key pillars of prevention, especially in children under five. But, although their use in Liberia is growing, less than half of this age group currently sleeps under one.
In health education sessions inside and outside the hospital, MSF encourages parents and carers to always use mosquito nets at home. Bed nets are even provided on admission to the hospital, to keep.
The health education also includes information about how to recognise that a child is ill and how dangerous convulsions can be without medical care.
For people who are worried about the cost of treatment, nurse Victoria sums it up:
“We always tell them ‘you are at the right place’ because MSF is free.”
MSF and malaria
Malaria is a deadly disease carried by Anopheles mosquitoes.
Every year, it kills around 430,000 people and infects more than 200 million. Ninety percent of these deaths occur in sub-Saharan Africa.
Despite malaria mortality rates falling by 25 percent since 2000, a child in Africa still dies every two minutes from malaria.